Image Defined Risk Factor
Image Defined Risk Factor refers to specific features identified through medical imaging that indicate an increased risk for disease progression, recurrence, or adverse outcomes. These factors are crucial in guiding clinical decisions and personalizing patient care.

Key Takeaways
- Image Defined Risk Factors (IDRFs) are imaging-based findings that predict disease risk.
- They are essential for accurate diagnosis, prognosis, and treatment planning in various medical conditions.
- Examples include tumor proximity to critical structures, vascular invasion, and specific lesion characteristics.
- IDRFs help clinicians stratify patients, select appropriate therapies, and monitor treatment effectiveness.
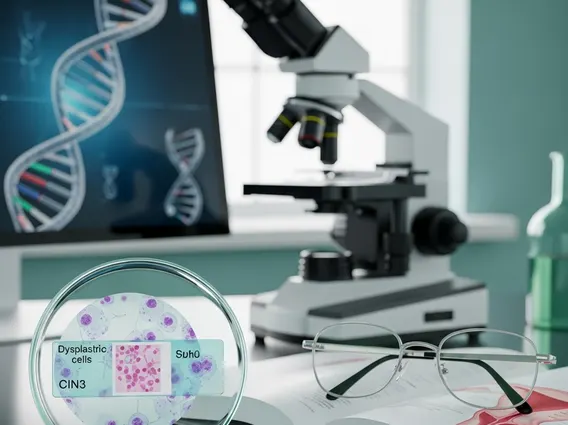
- Their identification relies on advanced imaging techniques like MRI, CT, and PET scans.
What is Image Defined Risk Factor?
An Image Defined Risk Factor (IDRF) refers to specific anatomical or pathological features identified through medical imaging studies that are associated with an increased likelihood of disease progression, recurrence, or complications. The image defined risk factor meaning encompasses findings that go beyond simple diagnosis, providing critical prognostic and predictive information. These factors are often subtle but carry significant weight in determining a patient’s risk profile and influencing treatment strategies. For instance, in oncology, an IDRF might indicate the extent of tumor invasion or its relationship to vital organs, which directly impacts surgical resectability and the need for adjuvant therapies.
IDRFs are identified using various imaging modalities, including Magnetic Resonance Imaging (MRI), Computed Tomography (CT), Positron Emission Tomography (PET), and ultrasound. The precise identification and characterization of these factors require expert radiological interpretation, often aided by advanced imaging sequences and post-processing techniques. Recognizing these risk factors early allows for more precise staging, better prediction of treatment response, and ultimately, improved patient outcomes.
Examples of Image Defined Risk Factors
The identification of specific imaging characteristics as risk factors is prevalent across numerous medical specialties, particularly in oncology. These factors provide tangible evidence that helps clinicians understand the aggressiveness of a disease and its potential impact.
Here are some common examples of Image Defined Risk Factors:
- Tumor Proximity to Critical Structures: In head and neck cancers, a tumor’s close proximity to major blood vessels or nerves, as seen on MRI or CT, can indicate a higher risk of surgical complications or incomplete resection.
- Vascular Invasion: The presence of tumor cells invading blood vessels, detectable through contrast-enhanced imaging, is a significant IDRF for metastasis and poorer prognosis in various cancers, such as pancreatic or liver cancer.
- Extracapsular Extension: In prostate cancer, imaging evidence of the tumor extending beyond the prostatic capsule is an IDRF indicating a higher risk of recurrence after surgery.
- Perineural Invasion: Imaging showing tumor cells tracking along nerves, particularly in cancers of the head, neck, and pancreas, is a strong indicator of increased local recurrence risk and distant metastasis.
- Specific Lesion Characteristics: Certain imaging features like irregular margins, heterogeneous enhancement, or rapid growth rate in a lesion can be IDRFs for malignancy, even in the absence of definitive biopsy results.
These examples highlight how imaging provides crucial insights that guide clinical decision-making beyond what physical examination or basic lab tests can offer.
Role of Image Defined Risk Factors in Patient Management
The role of image defined risk factors in patient management is multifaceted and profoundly impacts clinical decision-making. By providing a detailed anatomical and functional assessment of disease, IDRFs enable clinicians to stratify patients into different risk categories, leading to more personalized and effective treatment plans. This stratification is vital for determining the intensity of treatment, the choice of therapeutic modality (e.g., surgery, radiation, chemotherapy), and the frequency of follow-up.
For instance, in surgical oncology, the identification of an IDRF like vascular invasion might prompt a more extensive surgical approach or the addition of neoadjuvant therapy to shrink the tumor before surgery. Conversely, the absence of certain IDRFs might allow for a less aggressive, organ-preserving approach. According to the World Health Organization (WHO), accurate staging and risk stratification, heavily reliant on imaging, are critical for improving cancer survival rates globally. Furthermore, IDRFs are instrumental in monitoring disease progression or response to treatment. Changes in these imaging features over time can indicate whether a therapy is effective or if adjustments are needed, thereby optimizing patient care and improving long-term outcomes.