Cerebral Edema
Cerebral edema is a serious medical condition characterized by an accumulation of fluid within the brain, leading to increased intracranial pressure. This swelling can have profound and life-threatening consequences, impacting brain function and overall neurological health.

Key Takeaways
- Cerebral edema involves fluid accumulation in the brain, causing dangerous pressure.
- It can result from various causes, including trauma, stroke, tumors, and infections.
- Symptoms range from headaches and nausea to severe neurological deficits.
- Diagnosis relies on imaging like CT and MRI scans.
- Treatment focuses on reducing swelling and managing underlying causes, often requiring urgent medical intervention.
What is Cerebral Edema?
Cerebral Edema refers to the swelling of brain tissue due to increased fluid content, either intracellular or extracellular. Within the rigid skull, this fluid accumulation elevates intracranial pressure (ICP), which can compress delicate brain tissue, reduce blood flow, and potentially cause irreversible damage or death if not promptly managed. It is a critical condition demanding immediate attention.
Two primary types exist: vasogenic and cytotoxic. Vasogenic edema occurs when the blood-brain barrier is disrupted, allowing fluids and proteins to leak into the brain’s extracellular space. Cytotoxic edema results from cellular dysfunction, where brain cells swell due to failed ion pumps, often caused by ischemia or metabolic disturbances. Understanding what is Cerebral Edema and its types is crucial for effective diagnosis and treatment.
Causes, Symptoms, and Diagnosis of Cerebral Edema
Understanding the origins and manifestations of this condition is vital for timely intervention. Cerebral edema causes symptoms that vary widely based on severity, location, and underlying cause. Common causes include:
- Traumatic Brain Injury (TBI): Head impacts damage blood vessels and brain tissue.
- Stroke: Ischemic or hemorrhagic strokes disrupt blood flow, triggering edema.
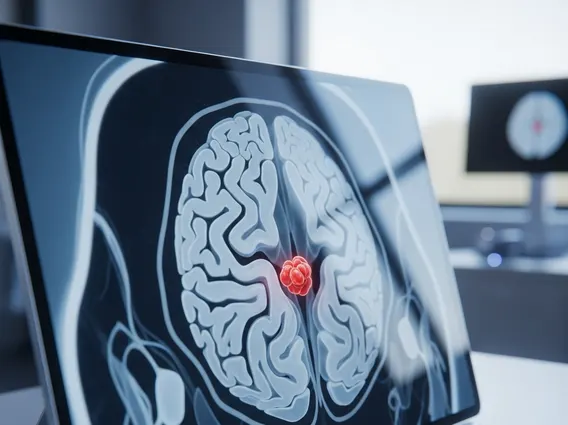
- Brain Tumors: Growing tumors exert pressure and disrupt the blood-brain barrier.
- Infections: Encephalitis or meningitis cause inflammation and brain swelling.
- High Altitude Cerebral Edema (HACE): A severe form of altitude sickness.
- Liver Failure: Severe liver dysfunction can lead to hepatic encephalopathy.
Symptoms often reflect increased intracranial pressure and impaired brain function, including: severe headache, nausea, vomiting, dizziness; confusion, disorientation, lethargy; seizures, weakness, numbness, vision changes (e.g., papilledema); difficulty speaking or understanding speech; and loss of consciousness or coma in severe cases.
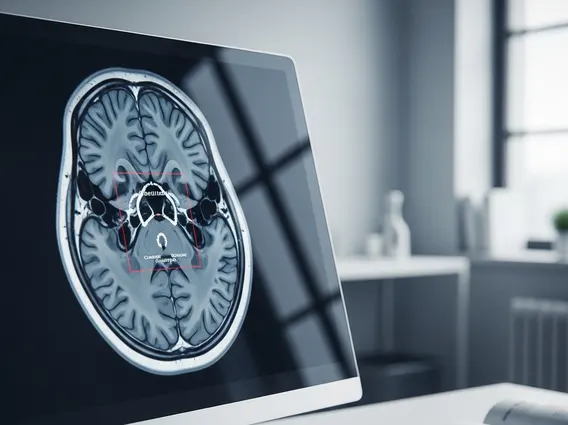
Diagnosing cerebral edema typically involves clinical evaluation and advanced imaging. A neurological examination assesses mental status, motor skills, and reflexes. Neuroimaging scans are primary diagnostic tools.
| Diagnostic Method | Description | Purpose |
|---|---|---|
| Computed Tomography (CT) Scan | Rapid X-ray imaging to detect acute swelling, bleeding, or mass lesions. | Quick assessment in emergencies; identifies major structural changes. |
| Magnetic Resonance Imaging (MRI) | Detailed imaging using magnetic fields and radio waves. | Provides higher resolution for subtle edema, ischemia, or tumors. |
| Intracranial Pressure (ICP) Monitoring | Direct measurement of pressure within the skull via a catheter. | Monitors pressure changes in critical care settings. |
Common Diagnostic Methods for Cerebral Edema
These studies pinpoint the edema’s location, extent, and underlying cause. Lumbar puncture may be performed for suspected infection, though often contraindicated with elevated ICP.
Cerebral Edema Treatment Options
Effective management of cerebral edema is critical to prevent permanent neurological damage. Cerebral edema treatment options vary based on cause, severity, and patient condition. Primary goals are to reduce intracranial pressure, maintain adequate cerebral blood flow, and address the root cause.
Initial management often involves supportive ICU care with close monitoring. Medical therapies include:
- Osmotic Diuretics: Mannitol or hypertonic saline draw fluid from brain tissue into the bloodstream.
- Corticosteroids: Dexamethasone reduces inflammation and stabilizes the blood-brain barrier, especially for tumor-associated edema.
- Barbiturate Coma: For severe cases, induced coma reduces brain metabolic demand and blood flow, lowering ICP.
- Therapeutic Hypothermia: Lowering body temperature can reduce brain metabolism and swelling.
Surgical interventions may be necessary:
- Ventriculostomy: Draining excess cerebrospinal fluid via a catheter to relieve pressure.
- Decompressive Craniectomy: Temporarily removing a skull section to allow brain expansion, reducing intracranial pressure, often a last resort.
- Removal of Mass Lesions: Surgical removal of tumors or hematomas to alleviate pressure.
Long-term prognosis depends on brain damage, treatment effectiveness, and underlying cause. Rehabilitation therapy (physical, occupational, speech) is crucial for recovering from neurological deficits. Information on supportive therapies does not replace professional medical treatment and should always be discussed with a healthcare provider.