Cerebellar Hemangioblastoma
Cerebellar Hemangioblastoma is a rare, non-cancerous tumor that originates in the cerebellum, the part of the brain responsible for coordination and balance. Understanding this condition is crucial for timely diagnosis and effective management.
Key Takeaways
- Cerebellar Hemangioblastoma is a rare, benign tumor primarily affecting the cerebellum, often associated with von Hippel-Lindau disease.
- Symptoms typically arise from increased intracranial pressure or direct compression of brain tissue, including headaches, nausea, and balance problems.
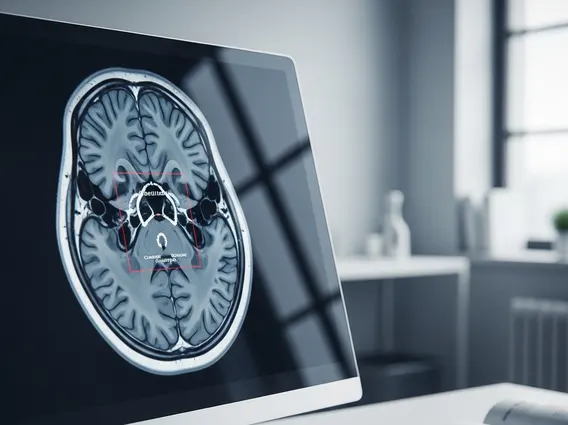
- Diagnosis involves imaging techniques like MRI and CT scans, often followed by genetic testing for VHL disease.
- Treatment primarily involves surgical removal, which is often curative, with radiation therapy as an alternative or supplementary option.
- Early detection and intervention are vital for improving patient outcomes and managing potential complications.
What is Cerebellar Hemangioblastoma and Its Causes?
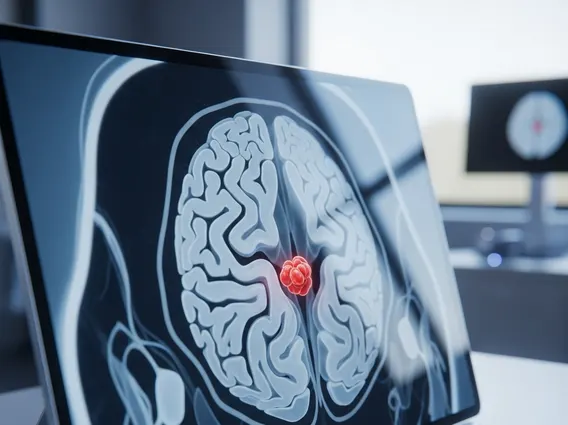
Cerebellar Hemangioblastoma is a type of benign (non-cancerous) tumor that forms from blood vessel cells within the cerebellum. These tumors are relatively rare, accounting for approximately 1-2.5% of all intracranial tumors and 7-12% of tumors found in the posterior fossa, the area at the back of the skull where the cerebellum is located. While benign, their growth can exert pressure on surrounding brain tissue, leading to significant neurological symptoms.
The primary causes of cerebellar hemangioblastoma are often linked to genetic factors. A significant proportion, estimated between 25% and 40%, are associated with von Hippel-Lindau (VHL) disease, a rare inherited disorder characterized by the growth of tumors and cysts in various parts of the body. In individuals with VHL disease, a mutation in the VHL gene (located on chromosome 3) leads to the abnormal proliferation of blood vessel cells. For cases not associated with VHL disease, known as sporadic hemangioblastomas, the exact cause is less clear but is also thought to involve somatic mutations in the VHL gene that occur spontaneously rather than being inherited. Environmental factors are not typically considered direct causes of these tumors.
Recognizing Cerebellar Hemangioblastoma Symptoms
The manifestation of cerebellar hemangioblastoma symptoms largely depends on the tumor’s size, location, and rate of growth, as well as the degree of pressure it exerts on the cerebellum and surrounding brain structures. Symptoms often develop gradually as the tumor enlarges, leading to a progressive decline in neurological function. These symptoms typically arise from two main mechanisms: increased intracranial pressure due to obstruction of cerebrospinal fluid flow (hydrocephalus) or direct compression of cerebellar tissue.
Common symptoms include:
- Headaches: Often severe, persistent, and worsening over time, particularly in the morning.
- Nausea and Vomiting: Frequently accompanying headaches, especially when intracranial pressure is elevated.
- Balance and Coordination Problems: Including ataxia (unsteady gait), dizziness, and difficulty with fine motor skills.
- Nystagmus: Involuntary, rapid eye movements.
- Dysarthria: Slurred speech due to impaired muscle control.
- Weakness or Numbness: In the limbs, though less common than other symptoms.
These symptoms can significantly impact a person’s quality of life and necessitate prompt medical evaluation. Diagnosis typically involves neurological examination and advanced imaging techniques such as Magnetic Resonance Imaging (MRI) and Computed Tomography (CT) scans, which can clearly visualize the tumor.
Treatment Approaches for Cerebellar Hemangioblastoma
The primary goal of cerebellar hemangioblastoma treatment is to remove the tumor and alleviate symptoms while preserving neurological function. Given that these tumors are typically benign, complete removal often results in a cure. The choice of treatment strategy depends on several factors, including the tumor’s size and location, the patient’s overall health, and whether the tumor is associated with VHL disease.
The most common and effective treatment is surgical resection. During surgery, neurosurgeons carefully remove the tumor, often with excellent outcomes. Advances in microsurgical techniques and intraoperative imaging have significantly improved the safety and efficacy of these procedures. For tumors that are small, asymptomatic, or located in areas that are difficult to access surgically, a “watch and wait” approach with regular imaging surveillance may be considered, especially in older patients or those with significant comorbidities.
In cases where complete surgical removal is not feasible or if there are multiple tumors (as often seen in VHL disease), radiation therapy may be used. Stereotactic radiosurgery (SRS) is a highly precise form of radiation therapy that delivers a concentrated dose of radiation to the tumor while minimizing exposure to surrounding healthy brain tissue. This can be an effective option for controlling tumor growth or treating residual tumors after surgery. For individuals with VHL disease, ongoing surveillance and management of other VHL-related manifestations are also critical. According to the National Cancer Institute, targeted therapies are also being explored for certain VHL-associated tumors, offering potential future treatment avenues.