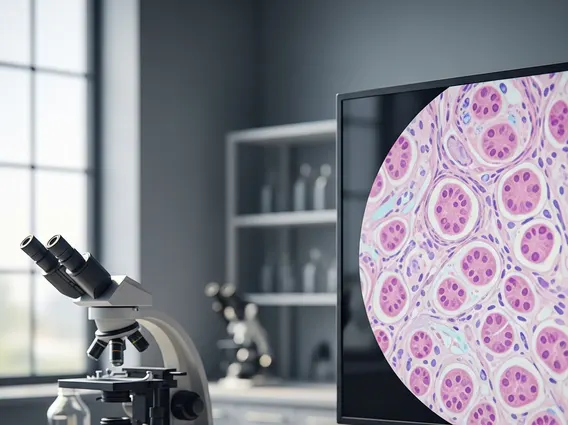
Granulosa Cell Tumor
Granulosa Cell Tumor is a rare type of ovarian cancer that originates from the granulosa cells of the ovary. These tumors are unique due to their ability to produce hormones, primarily estrogen, which can lead to a variety of clinical manifestations.
Key Takeaways
- Granulosa Cell Tumor is a rare ovarian cancer known for estrogen production.
- Symptoms often relate to hormonal imbalances, such as abnormal bleeding or precocious puberty.
- Diagnosis involves imaging, tumor markers, and tissue biopsy.
- Treatment primarily consists of surgery, sometimes followed by chemotherapy or radiation.
- Prognosis is generally favorable, but recurrence is possible, necessitating long-term monitoring.
What is Granulosa Cell Tumor?
A Granulosa Cell Tumor (GCT) is a type of sex cord-stromal tumor that develops in the ovaries. These tumors are relatively rare, accounting for approximately 2-5% of all ovarian cancers. What makes them distinct is their capacity to produce steroid hormones, predominantly estrogen, which can significantly impact a patient’s endocrine system. The clinical presentation of GCTs can vary widely depending on the patient’s age and the amount of hormone produced, making early detection crucial.
The term granulosa cell tumor explained refers to a neoplasm arising from the granulosa cells, which are integral to ovarian follicle development and hormone production. These tumors can occur at any age, from childhood to post-menopause, though they are most commonly found in adult women. According to the American Cancer Society, the average age of diagnosis is around 50-55 years, but juvenile forms also exist, presenting with distinct characteristics.
Recognizing Granulosa Cell Tumor: Symptoms and Causes
The granulosa cell tumor symptoms and signs are largely influenced by the tumor’s estrogen production. In premenopausal women, excessive estrogen can lead to irregular or heavy menstrual bleeding, amenorrhea (absence of menstruation), or postmenopausal bleeding. In children, it may cause precocious puberty, characterized by early breast development and menstruation. Other non-specific symptoms can include abdominal pain, bloating, or a palpable abdominal mass, which are common to many ovarian conditions. These symptoms often prompt medical evaluation.
While the exact causes of granulosa cell tumor are not fully understood, research suggests a combination of genetic and environmental factors may play a role. A specific genetic mutation, FOXL2 C134W, has been identified in a significant percentage of adult GCTs, indicating a potential genetic predisposition. However, most cases are sporadic, meaning they occur without a clear inherited pattern. Unlike some other cancers, there are no well-established modifiable risk factors like diet or lifestyle directly linked to GCT development, making prevention challenging.
Common symptoms associated with Granulosa Cell Tumor include:
- Abnormal uterine bleeding (heavy, irregular, or postmenopausal)
- Precocious puberty in young girls
- Abdominal pain or discomfort
- Abdominal distension or bloating
- Palpable abdominal or pelvic mass
Diagnosis and Treatment of Granulosa Cell Tumor
The approach to granulosa cell tumor diagnosis and treatment involves several steps. Diagnosis typically begins with a thorough physical examination and a detailed medical history. Imaging studies, such as pelvic ultrasound, CT scans, or MRI, are crucial for visualizing the ovarian mass and assessing its characteristics. Blood tests for tumor markers, particularly inhibin A and B, and anti-Müllerian hormone (AMH), are highly valuable as these markers are often elevated in GCT patients. However, a definitive diagnosis requires a biopsy and histopathological examination of the tumor tissue, usually obtained during surgery.
Treatment for Granulosa Cell Tumor is primarily surgical. The extent of surgery depends on the tumor’s stage, the patient’s age, and their desire for future fertility. For early-stage disease, fertility-sparing surgery (removing only the affected ovary and fallopian tube) may be an option for younger patients. For more advanced stages or in postmenopausal women, a total hysterectomy with bilateral salpingo-oophorectomy (removal of the uterus, both ovaries, and fallopian tubes) is usually performed. Adjuvant therapies, such as chemotherapy or radiation, may be considered for advanced or recurrent disease, though their role is still being refined. Regular follow-up with imaging and tumor marker monitoring is essential due to the potential for late recurrence.