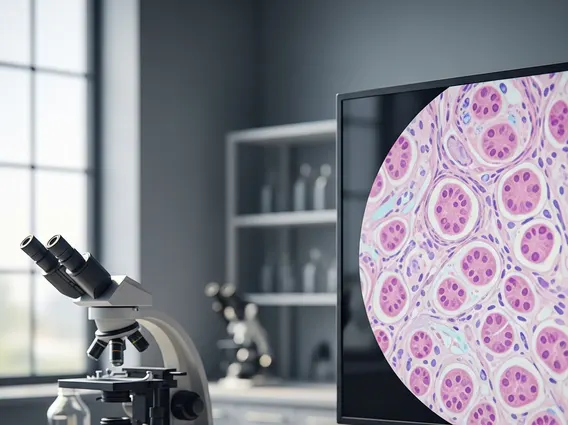
Gastrointestinal Neuroendocrine Tumor
Gastrointestinal neuroendocrine tumors (GI NETs) are a diverse group of cancers that originate in the neuroendocrine cells of the digestive tract. These cells have characteristics of both nerve cells and hormone-producing endocrine cells, making GI NETs unique in their behavior and presentation.
Key Takeaways
- Gastrointestinal Neuroendocrine Tumor (GI NET) is a rare cancer arising from specialized cells in the digestive system that produce hormones.
- Symptoms of GI neuroendocrine tumor can vary widely depending on the tumor’s location and whether it produces hormones, often leading to delayed diagnosis.
- The exact causes of gastrointestinal NET are not fully understood, but genetic factors and certain medical conditions may increase risk.
- Treatment for GI neuroendocrine tumor is highly individualized, involving surgery, targeted therapies, and other specialized approaches.
- Early detection and a multidisciplinary approach are crucial for managing GI NETs and improving patient outcomes.
What is a Gastrointestinal Neuroendocrine Tumor (GI NET)?
A Gastrointestinal Neuroendocrine Tumor (GI NET) is a type of cancer that forms in the neuroendocrine cells found throughout the gastrointestinal tract, including the stomach, small intestine, appendix, colon, and rectum. These cells are unique because they share features with both nerve cells and hormone-producing endocrine cells. Consequently, GI NETs can produce and release hormones into the bloodstream, leading to a variety of symptoms known as carcinoid syndrome in some cases. GI NETs are considered relatively rare, accounting for less than 2% of all gastrointestinal malignancies, but their incidence has been increasing over recent decades, partly due to improved diagnostic techniques. According to the National Cancer Institute, the incidence rate of neuroendocrine tumors (NETs) has risen significantly, highlighting the importance of understanding these complex cancers.
The behavior of a GI NET can range from slow-growing and relatively benign to aggressive and metastatic, depending on factors such as its location, size, and grade. They are often classified based on their primary site of origin and whether they are functional (producing hormones) or non-functional. Understanding the specific characteristics of a GI NET is critical for accurate diagnosis and effective management.
Symptoms and Causes of Gastrointestinal Neuroendocrine Tumors
The symptoms of GI neuroendocrine tumor can be highly variable and non-specific, often leading to a delayed diagnosis. This variability is largely due to the tumor’s location within the GI tract and whether it is producing hormones. When a GI NET produces excess hormones, it can lead to a condition called carcinoid syndrome, characterized by a distinct set of symptoms. However, many GI NETs are non-functional and may only cause symptoms as they grow and press on surrounding organs.
Common symptoms may include:
- Abdominal pain or discomfort
- Changes in bowel habits (diarrhea or constipation)
- Nausea and vomiting
- Unexplained weight loss
- Fatigue
- Gastrointestinal bleeding
- Symptoms of carcinoid syndrome: flushing, diarrhea, wheezing, and rapid heart rate (if the tumor is hormone-producing)
The exact causes of gastrointestinal NET are not fully understood, and in most cases, they occur sporadically without a clear identifiable cause. However, certain risk factors and genetic predispositions have been identified. These include inherited genetic syndromes such as Multiple Endocrine Neoplasia type 1 (MEN1), Von Hippel-Lindau disease, Neurofibromatosis type 1, and Tuberous Sclerosis Complex. While these genetic conditions increase the risk, they account for a small percentage of all GI NET cases. Lifestyle factors and environmental exposures are not strongly linked to the development of GI NETs, unlike many other common cancers. Research continues to explore the molecular pathways and genetic mutations that contribute to the formation and progression of these tumors.
Treatment Options for Gastrointestinal Neuroendocrine Tumors
The treatment for GI neuroendocrine tumor is highly individualized and depends on several factors, including the tumor’s location, size, grade, hormone production, and whether it has spread to other parts of the body. A multidisciplinary team of specialists, including oncologists, surgeons, endocrinologists, and radiologists, typically collaborates to develop the most appropriate treatment plan for each patient.
Surgical removal is often the primary treatment for localized GI NETs, aiming to remove the tumor and any affected lymph nodes. For tumors that have spread or are inoperable, various other therapies may be employed:
| Treatment Type | Description |
|---|---|
| Somatostatin Analogs (SSAs) | Medications like octreotide and lanreotide that help control hormone-related symptoms and can slow tumor growth, especially for functional tumors. |
| Targeted Therapies | Drugs such as everolimus and sunitinib that specifically target pathways involved in tumor growth and survival, often used for advanced or progressive disease. |
| Chemotherapy | Used for more aggressive or poorly differentiated GI NETs, aiming to kill rapidly dividing cancer cells throughout the body. |
| Radionuclide Therapy (PRRT) | Peptide Receptor Radionuclide Therapy (e.g., Lutathera) uses a radioactive substance linked to a somatostatin analog to deliver radiation directly to tumor cells expressing somatostatin receptors. |
| Liver-Directed Therapies | For tumors that have spread to the liver, treatments like embolization, radiofrequency ablation, or chemoembolization may be used to control liver metastases. |
Ongoing monitoring and surveillance are crucial after initial treatment to detect any recurrence or progression. This often involves regular imaging scans, blood tests for tumor markers, and clinical evaluations. The goal of treatment is not only to eliminate or control the tumor but also to manage symptoms and improve the patient’s quality of life.