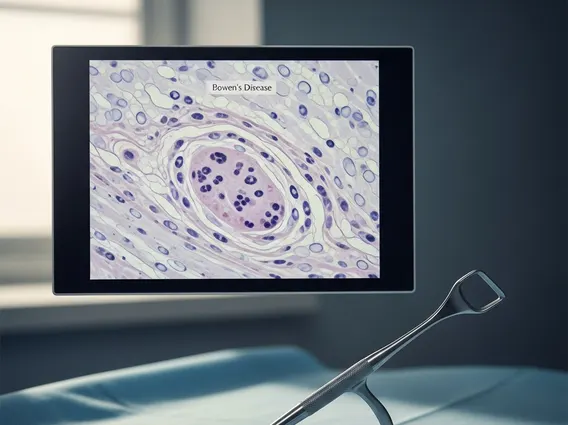
Stage 0 Colorectal Carcinoma In Situ
Stage 0 Colorectal Carcinoma In Situ represents the earliest form of colorectal cancer, where abnormal cells are confined to the innermost layer of the colon or rectum. Understanding this initial stage is crucial for effective prevention and treatment.
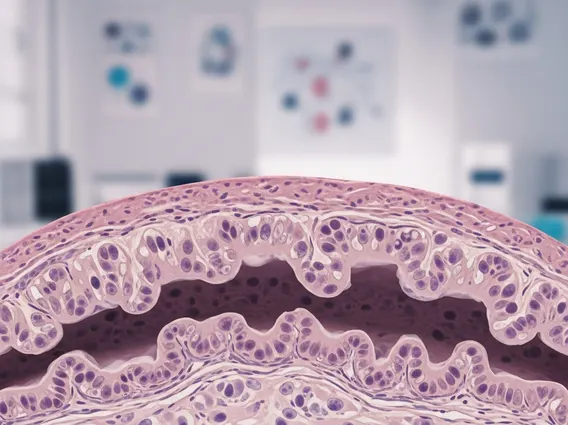
Key Takeaways
- Stage 0 Colorectal Carcinoma In Situ is the earliest stage of colorectal cancer, involving abnormal cells only in the mucosa.
- It is highly curable because the abnormal cells have not invaded deeper tissues.
- Symptoms are typically absent, making regular screening vital for detection.
- Treatment often involves localized removal of the abnormal tissue, such as polypectomy.
- Early detection through colonoscopy significantly improves prognosis.
What is Stage 0 Colorectal Carcinoma In Situ?
Stage 0 Colorectal Carcinoma In Situ refers to the earliest form of colorectal cancer, also known as high-grade dysplasia or intramucosal carcinoma. In this stage, abnormal cells are found only in the innermost lining of the colon or rectum, called the mucosa, and have not yet invaded the deeper layers of tissue. This non-invasive characteristic is what distinguishes it from more advanced stages of colorectal cancer. The term “in situ” literally means “in its original place,” indicating that the cancerous cells are confined and have not spread.
The colorectal carcinoma in situ definition emphasizes that these cells have not breached the muscularis mucosa, a thin layer separating the mucosa from the submucosa. Because the abnormal cells are contained within the mucosa, they do not have access to blood vessels or lymphatic channels, meaning they cannot spread to other parts of the body. This makes Stage 0 highly curable, often through minimally invasive procedures. According to the American Cancer Society, early detection of colorectal cancer, including in situ cases, significantly improves survival rates.
Symptoms of Stage 0 Colorectal Carcinoma In Situ
Stage 0 colorectal cancer in situ symptoms are typically non-existent, making this condition particularly challenging to detect without regular screening. Because the abnormal cells are confined to the surface lining and have not invaded deeper tissues or caused significant tissue damage, they usually do not produce any noticeable signs or symptoms. This asymptomatic nature underscores the importance of routine colorectal cancer screenings, such as colonoscopies, especially for individuals over the age of 45 or those with specific risk factors.
When symptoms do occur in very rare instances, they are often vague and can be attributed to other, less serious conditions. These might include minor changes in bowel habits (e.g., slight constipation or diarrhea), or rectal bleeding (often microscopic and not visible to the naked eye). However, it is crucial to reiterate that these symptoms are highly unlikely at Stage 0 and are far more common in later stages of colorectal cancer. The absence of symptoms highlights why screening is the primary method for identifying Stage 0 colorectal carcinoma in situ, allowing for early intervention before the condition progresses.
Treatment Options for Stage 0 Colorectal Carcinoma
Treatment for Stage 0 Colorectal Carcinoma is highly effective due to the localized nature of the abnormal cells. The primary goal is to completely remove the cancerous tissue while preserving as much healthy colon or rectal tissue as possible. Since the cells have not invaded beyond the mucosa, extensive surgery or systemic treatments like chemotherapy or radiation are typically not required.
Common treatment approaches include:
- Polypectomy: This is the most common treatment if the carcinoma in situ is found within a polyp. During a colonoscopy, the doctor can remove the polyp using a wire loop and electrical current. This procedure is minimally invasive and often curative.
- Endoscopic Mucosal Resection (EMR): For larger or flatter areas of carcinoma in situ, EMR may be performed. This involves injecting a solution under the abnormal tissue to lift it, making it easier to remove endoscopically.
- Endoscopic Submucosal Dissection (ESD): In some complex cases, ESD might be used to remove larger lesions en bloc (in one piece), offering a more precise removal.
- Local Excision: If the lesion cannot be completely removed endoscopically, a small surgical procedure might be performed to excise the affected area. This is typically done for rectal lesions that are easily accessible.
The choice of treatment depends on factors such as the size, location, and characteristics of the lesion. Following treatment, regular surveillance colonoscopies are recommended to monitor for recurrence or the development of new polyps, ensuring long-term health and preventing progression.