Fallopian Tube Cancer
Fallopian tube cancer is a rare gynecologic malignancy that originates in the fallopian tubes, which are the conduits connecting the ovaries to the uterus. Understanding this condition is crucial for early detection and effective management.

Key Takeaways
- Fallopian tube cancer is a rare cancer originating in the tubes connecting ovaries to the uterus.
- Symptoms are often vague and can mimic other conditions, making early diagnosis challenging.
- Risk factors include genetic mutations (like BRCA1/2) and a personal history of ovarian or breast cancer.
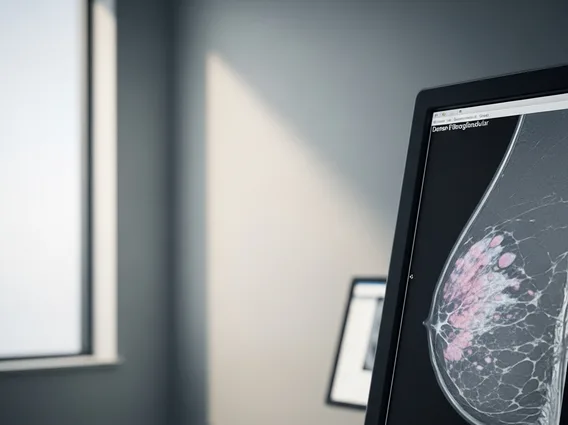
- Diagnosis typically involves imaging, blood tests, and surgical biopsy.
- Treatment primarily involves surgery, often followed by chemotherapy.
What is Fallopian Tube Cancer?
Fallopian tube cancer refers to a rare type of cancer that begins in the fallopian tubes, the two slender tubes that transport eggs from the ovaries to the uterus. This malignancy is often considered similar to ovarian cancer due to their shared embryological origin and similar treatment approaches, though it is a distinct condition. It represents a small percentage of all gynecological cancers, with an incidence rate significantly lower than that of ovarian or uterine cancer. According to the American Cancer Society, primary fallopian tube cancer is extremely rare, often grouped with ovarian and primary peritoneal cancers due to their similar characteristics and treatment protocols.
Most fallopian tube cancers are adenocarcinomas, meaning they originate in the glandular cells lining the fallopian tubes. These cancers can spread to nearby organs, such as the ovaries, uterus, and peritoneum, and can also metastasize to distant sites through the bloodstream or lymphatic system. Early detection is challenging because the symptoms are often non-specific and can be mistaken for more common, benign conditions.
Symptoms and Causes of Fallopian Tube Cancer
Recognizing the signs of this rare cancer is vital, although symptoms can be subtle and mimic other conditions. Fallopian tube cancer symptoms often develop as the tumor grows and include:
- Pelvic pain or pressure: A persistent discomfort or feeling of fullness in the lower abdomen.
- Abnormal vaginal bleeding: Bleeding outside of menstrual periods, after menopause, or unusually heavy periods.
- Vaginal discharge: A watery, clear, or blood-tinged discharge, sometimes described as “hydrops tubae profluens” (a classic but rare symptom involving intermittent discharge of fluid from the fallopian tube).
- Abdominal bloating or distension: A persistent feeling of swelling or an increase in abdominal size.
- Changes in bowel or bladder habits: Such as frequent urination or constipation.
The exact causes of fallopian tube cancer are not fully understood, but several risk factors have been identified. These factors increase an individual’s likelihood of developing the disease, though many people with these risks never develop cancer, and some without them do. Key risk factors include:
- Genetic Mutations: Inherited mutations in genes like BRCA1 and BRCA2 are significant risk factors, as they are for ovarian and breast cancer.
- Family History: A personal or family history of ovarian, breast, or colorectal cancer can increase risk.
- Age: The risk generally increases with age, most commonly diagnosed in women over 50.
- Endometriosis: A condition where tissue similar to the lining of the uterus grows outside the uterus.
- Nulliparity: Women who have never given birth may have a slightly increased risk.
- Infertility: Some studies suggest a link between infertility and an increased risk of fallopian tube cancer.
It’s important to note that having one or more risk factors does not mean an individual will develop fallopian tube cancer, but it warrants discussion with a healthcare provider.
Fallopian Tube Cancer Treatment Approaches
The primary goal of fallopian tube cancer treatment is to remove as much of the cancer as possible and prevent its recurrence or spread. Treatment plans are highly individualized, depending on the stage of the cancer, the patient’s overall health, and other factors. The mainstays of treatment typically involve surgery, often followed by chemotherapy.
- Surgery: This is usually the first and most crucial step. The standard surgical procedure is a total hysterectomy (removal of the uterus), bilateral salpingo-oophorectomy (removal of both fallopian tubes and ovaries), and omentectomy (removal of the omentum, a fatty tissue in the abdomen). Lymph node dissection and removal of any visible tumors (debulking) are also performed to stage the cancer and reduce tumor burden.
- Chemotherapy: After surgery, chemotherapy is often administered to kill any remaining cancer cells and reduce the risk of recurrence. Common chemotherapy regimens involve platinum-based drugs (like carboplatin) and taxanes (like paclitaxel), similar to those used for ovarian cancer. Chemotherapy may be given intravenously or, in some cases, intraperitoneally (directly into the abdominal cavity).
- Targeted Therapy: For some patients, targeted therapies that focus on specific vulnerabilities of cancer cells may be an option, particularly for recurrent or advanced disease. These drugs work differently from traditional chemotherapy and often have fewer side effects.
- Radiation Therapy: While less common for primary fallopian tube cancer, radiation therapy may be used in specific situations, such as to manage localized recurrence or to alleviate symptoms.
Regular follow-up appointments, including physical examinations, blood tests (such as CA-125 levels), and imaging scans, are essential after treatment to monitor for any signs of recurrence. Early diagnosis and a comprehensive, multidisciplinary approach to treatment offer the best prognosis for individuals with fallopian tube cancer.