Benign Proliferative Breast Disease
Benign Proliferative Breast Disease refers to a group of non-cancerous conditions characterized by an overgrowth of cells in the breast tissue. While these conditions are not malignant, some types may indicate an increased risk for developing breast cancer in the future, making accurate diagnosis and monitoring crucial.

Key Takeaways
- Benign Proliferative Breast Disease involves non-cancerous cell overgrowth in the breast.
- It often presents without specific symptoms and is frequently discovered during routine screenings or biopsies.
- While benign, certain types, like atypical hyperplasia, can elevate future breast cancer risk.
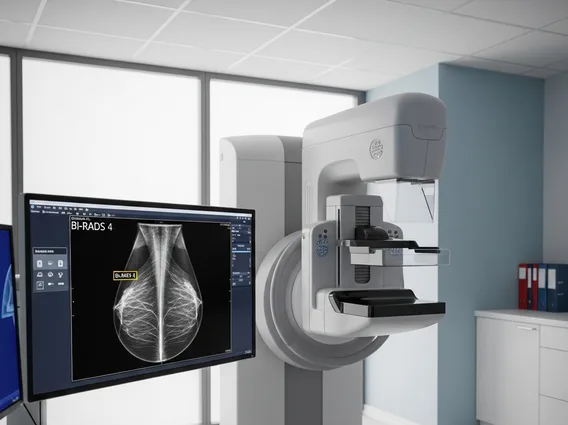
- Diagnosis typically involves imaging (mammography, ultrasound) followed by a biopsy for definitive confirmation.
- Regular follow-up and personalized management plans are essential for individuals diagnosed with these conditions.
What is Benign Proliferative Breast Disease?
Benign Proliferative Breast Disease is a broad category encompassing several non-cancerous conditions where there is an increase in the number of cells within the breast ducts or lobules. These cellular changes are not malignant, meaning they do not spread to other parts of the body. However, the presence of these proliferative changes signifies abnormal cell growth, which can sometimes be a precursor to or an indicator of an elevated risk for breast cancer.
These conditions are classified based on the specific cellular characteristics observed under a microscope. Understanding the type of proliferative change is important for risk assessment and management. Common types include:
- Usual Ductal Hyperplasia (UDH): An increase in the number of cells lining the milk ducts, which are typically normal in appearance. It is a common finding and carries a slightly increased risk of breast cancer.
- Sclerosing Adenosis: Characterized by an increase in the number of glandular components (lobules) and fibrous tissue, often distorting the breast architecture.
- Radial Scar (Complex Sclerosing Lesion): A star-shaped lesion that can mimic cancer on imaging due to its radiating appearance, involving both proliferative and sclerotic changes.
- Atypical Ductal Hyperplasia (ADH): Involves cell growth in the ducts that have some, but not all, features of ductal carcinoma in situ (DCIS), a non-invasive form of breast cancer. ADH significantly increases the risk of future breast cancer.
- Atypical Lobular Hyperplasia (ALH): Similar to ADH but involves the lobules (milk-producing glands). It also indicates an increased risk for breast cancer.
According to the American Cancer Society, certain types of benign proliferative breast disease, particularly atypical hyperplasia (ADH and ALH), can increase a woman’s risk of developing breast cancer by 4 to 5 times compared to women without these conditions.
Symptoms and Causes of Benign Proliferative Breast Disease
Many individuals with benign proliferative breast disease symptoms do not experience any noticeable signs or symptoms. These conditions are frequently discovered incidentally during routine mammograms, breast ultrasounds, or breast biopsies performed for other reasons, such as evaluating a suspicious lump or an abnormal imaging finding. When symptoms do occur, they are often non-specific and can include:
- A palpable breast lump or area of thickening.
- Breast pain or tenderness.
- Nipple discharge.
- Changes in breast size or shape.
It is important to note that these symptoms are common to many benign breast conditions and do not automatically indicate a proliferative disease. Any persistent breast changes should always be evaluated by a healthcare professional.
The exact causes of benign proliferative breast disease are not fully understood, but they are believed to involve a combination of hormonal, genetic, and environmental factors. Hormonal fluctuations, particularly exposure to estrogen, are thought to play a significant role, as breast tissue is highly sensitive to hormones. Other potential contributing factors may include family history of breast cancer, certain genetic predispositions, and lifestyle choices, though more research is needed to establish definitive causal links. These conditions represent a spectrum of cellular changes, reflecting the complex interplay of factors influencing breast health.
Diagnosing Benign Proliferative Breast Disease
The process of benign proliferative breast disease diagnosis typically begins with a thorough clinical breast examination and imaging studies. If a suspicious area is identified through a mammogram, ultrasound, or magnetic resonance imaging (MRI), further diagnostic steps are usually recommended. These imaging techniques can help characterize the abnormality but cannot definitively distinguish between benign and malignant conditions.
The definitive diagnosis of benign proliferative breast disease requires a tissue biopsy. During a biopsy, a small sample of breast tissue is removed and examined by a pathologist under a microscope. There are several types of biopsies:
- Core Needle Biopsy: A hollow needle is used to extract several tissue samples. This is often performed with imaging guidance (ultrasound or mammography) to ensure accuracy.
- Vacuum-Assisted Biopsy: Similar to a core needle biopsy but uses a vacuum to collect larger tissue samples through a single incision.
- Surgical Biopsy (Excisional Biopsy): In some cases, the entire suspicious area or mass is surgically removed for examination.
Once the biopsy results confirm benign proliferative changes, the management plan will depend on the specific type of disease identified and the individual’s overall risk factors. For conditions like atypical hyperplasia, healthcare providers often recommend increased surveillance, which may include more frequent clinical exams and imaging, and sometimes risk-reducing medications or genetic counseling, to monitor for any progression or new developments.