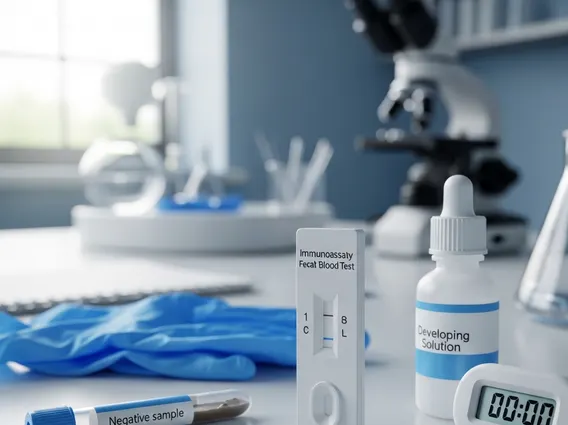
Immunoassay
Immunoassays are powerful biochemical tests used across various medical and research fields. These assays leverage the highly specific binding between antibodies and antigens to detect or quantify substances in biological samples.

Key Takeaways
- Immunoassays are laboratory techniques that detect or measure specific substances (analytes) using antigen-antibody reactions.
- They are based on the principle of specific molecular recognition, where an antibody binds precisely to its target antigen.
- Common techniques include ELISA, radioimmunoassay (RIA), and chemiluminescence immunoassay (CLIA), each offering distinct advantages in sensitivity and application.
- Immunoassays are crucial in clinical diagnostics for disease detection, therapeutic drug monitoring, and screening for various conditions.
- Their applications span from infectious disease diagnosis and cancer marker detection to allergy testing and hormone level assessment.
What is Immunoassay?
Immunoassay refers to a biochemical test that measures the presence or concentration of a macromolecule or a small molecule in a solution through the use of an antibody or antigen. This analytical method relies on the unique ability of an antibody to recognize and bind specifically to its corresponding antigen. The strength and specificity of this interaction form the fundamental basis for detecting a wide range of substances, from hormones and proteins to infectious agents and therapeutic drugs, within biological samples such as blood, urine, or saliva.
These tests are indispensable tools in modern medicine, offering high sensitivity and specificity for various diagnostic and monitoring purposes. The development of immunoassays revolutionized clinical diagnostics by providing rapid and accurate results, enabling timely medical interventions and improving patient outcomes. Their utility extends beyond diagnostics into research, environmental monitoring, and food safety testing.
Immunoassay Principles, Techniques, and Clinical Applications
Understanding how immunoassays work involves appreciating the core principle of antigen-antibody specificity. In essence, an immunoassay utilizes a labeled component (either the antigen or the antibody) to create a detectable signal when the binding event occurs. This label can be an enzyme, a fluorescent molecule, a radioactive isotope, or a chemiluminescent compound, allowing for the quantification of the target analyte. The signal generated is directly proportional to the amount of the substance being measured, providing quantitative or qualitative results.
Several types of immunoassay techniques have been developed, each with specific advantages and applications. These techniques vary in their format, labeling methods, and detection systems, but all share the common foundation of antigen-antibody recognition.
- Enzyme-Linked Immunosorbent Assay (ELISA): This widely used technique employs an enzyme conjugated to an antibody or antigen. The enzyme reacts with a substrate to produce a colored, fluorescent, or luminescent product, which is then measured. ELISA can be configured in various formats, including direct, indirect, sandwich, and competitive assays, making it highly versatile for detecting both antigens and antibodies.
- Radioimmunoassay (RIA): RIA uses radioactive isotopes as labels. While highly sensitive, its use has decreased due to concerns about radioactivity and the availability of safer alternatives.
- Chemiluminescence Immunoassay (CLIA): CLIA utilizes chemiluminescent labels that emit light upon chemical reaction. This method offers excellent sensitivity and a broad dynamic range, making it popular in automated clinical analyzers.
- Fluorescence Immunoassay (FIA): FIA employs fluorescent labels that emit light at a specific wavelength when excited by another light source.
The immunoassay principles and applications are vast and critical in clinical diagnostics. These tests are routinely used for:
- Infectious Disease Diagnosis: Detecting antibodies against pathogens (e.g., HIV, hepatitis viruses) or the pathogens themselves (e.g., bacterial antigens).
- Hormone Level Measurement: Quantifying hormones like thyroid hormones, reproductive hormones, and cortisol for endocrine disorder diagnosis and monitoring.
- Cancer Marker Detection: Identifying tumor markers (e.g., PSA for prostate cancer, CEA for colorectal cancer) to aid in diagnosis, prognosis, and monitoring treatment response.
- Therapeutic Drug Monitoring (TDM): Measuring drug concentrations in patient samples to optimize dosing and prevent toxicity, especially for drugs with narrow therapeutic windows.
- Allergy Testing: Detecting allergen-specific IgE antibodies to identify triggers for allergic reactions.
According to the World Health Organization (WHO), diagnostic tools like immunoassays are fundamental for effective disease surveillance and public health initiatives globally. Their ability to provide accurate and timely information empowers healthcare professionals to make informed decisions, leading to better patient management and disease control.