Meningioma
Meningioma is a common type of primary brain tumor that originates in the meninges, the protective layers surrounding the brain and spinal cord. While often benign, its location and size can significantly impact neurological function and overall health.

Key Takeaways
- Meningiomas are tumors arising from the meninges, the membranes covering the brain and spinal cord.
- They are among the most common primary brain tumors, with the majority being non-cancerous (benign).
- Symptoms vary widely depending on the tumor’s size and location, often including headaches, seizures, or vision problems.
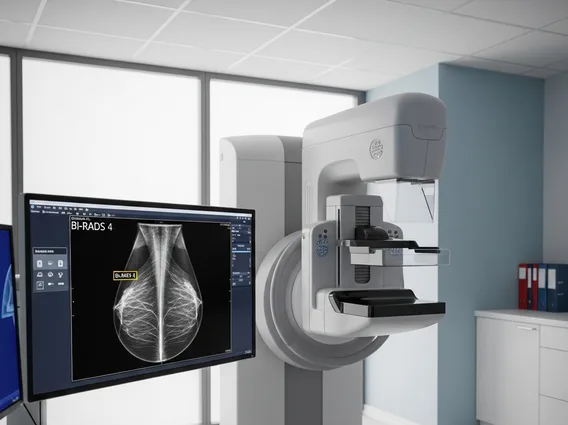
- Diagnosis typically involves imaging tests like MRI, often confirmed by biopsy.
- Treatment options range from watchful waiting to surgery and radiation, with a generally favorable prognosis for benign cases.
What is Meningioma: Understanding This Brain Tumor
Meningioma refers to a tumor that develops from the meninges, the three layers of tissue that encase and protect the brain and spinal cord. These tumors are typically slow-growing and are among the most common types of primary brain tumors, accounting for approximately 30-37% of all primary central nervous system tumors, according to the American Association of Neurological Surgeons (AANS). The vast majority of meningiomas are benign (non-cancerous), meaning they do not spread to other parts of the body. However, even a benign meningioma brain tumor can cause significant health issues if it grows large enough to press on the brain, nerves, or blood vessels, leading to various neurological symptoms.
Meningiomas are classified into three grades by the World Health Organization (WHO). Grade I meningiomas are benign and slow-growing. Grade II (atypical) meningiomas grow faster and have a higher chance of recurrence. Grade III (anaplastic or malignant) meningiomas are rare, fast-growing, and cancerous, with a higher likelihood of spreading within the central nervous system. The exact cause of meningiomas is often unknown, but risk factors can include exposure to radiation, certain genetic conditions like neurofibromatosis type 2, and hormonal factors, as they are more common in women.
Meningioma Symptoms and Diagnosis
The symptoms of a meningioma can vary widely depending on the tumor’s size, growth rate, and precise location within the brain or spinal cord. Because these tumors often grow slowly, symptoms may develop gradually over time and can be subtle initially. Some individuals may not experience any symptoms, with the tumor being discovered incidentally during imaging for another condition.
Common symptoms associated with meningioma include:
- Headaches that worsen over time
- Seizures
- Vision changes (e.g., blurred vision, double vision, loss of peripheral vision)
- Hearing loss or ringing in the ears (tinnitus)
- Weakness or numbness in the limbs
- Changes in personality or cognitive function
- Speech difficulties
The diagnosis of meningioma symptoms and diagnosis typically begins with a neurological examination to assess reflexes, vision, hearing, balance, and coordination. If a tumor is suspected, advanced imaging techniques are crucial. Magnetic Resonance Imaging (MRI) with contrast is the most effective diagnostic tool, providing detailed images of the brain and spinal cord. Computed Tomography (CT) scans may also be used, particularly to identify calcifications often present in meningiomas. In some cases, a biopsy—the surgical removal of a small tissue sample for microscopic examination—is performed to confirm the diagnosis and determine the tumor’s grade.
Meningioma Treatment Options and Prognosis
The approach to meningioma treatment options explained is highly individualized, depending on factors such as the tumor’s size, location, grade, the patient’s age, overall health, and the severity of symptoms. For small, asymptomatic, or slow-growing meningiomas, a “watchful waiting” approach may be recommended. This involves regular MRI scans to monitor the tumor’s growth, avoiding immediate intervention if it poses no immediate threat.
When treatment is necessary, surgical removal is often the primary option. The goal of surgery is to remove as much of the tumor as safely possible without damaging surrounding healthy brain tissue. Complete surgical removal, especially for benign tumors, can often lead to a cure. However, if the tumor is in a difficult-to-reach area or is close to critical structures, complete removal may not be feasible. In such cases, or for recurrent tumors, radiation therapy may be used. This can involve conventional external beam radiation or more focused techniques like stereotactic radiosurgery, which delivers a high dose of radiation precisely to the tumor while minimizing exposure to healthy tissue.
The benign meningioma prognosis and outlook are generally favorable, especially for Grade I tumors that can be completely removed surgically. Many individuals live long, healthy lives after treatment. Even for tumors that cannot be fully removed, management strategies can effectively control growth and symptoms. Regular follow-up appointments and imaging are essential to monitor for recurrence or new growth. While malignant meningiomas have a less favorable prognosis, advancements in multimodal treatment approaches continue to improve outcomes for all grades.