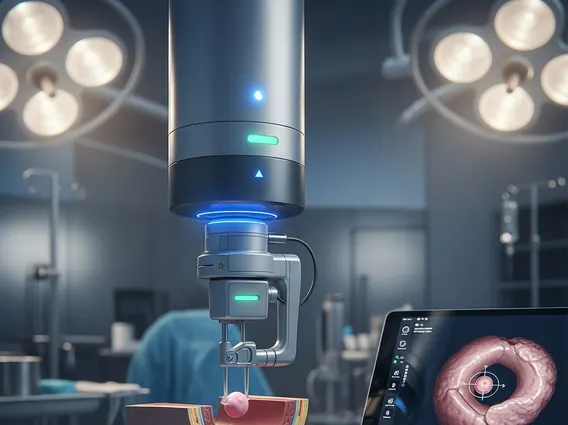
Mastitis
Mastitis is an inflammatory condition of the breast, often accompanied by infection. While it can affect anyone, it is most commonly observed in breastfeeding women.
Key Takeaways
- Mastitis is an inflammation of breast tissue, frequently caused by bacterial infection or blocked milk ducts.
- Common symptoms include breast pain, swelling, redness, warmth, and flu-like symptoms.
- It primarily affects breastfeeding women but can occur in non-lactating individuals.
- Treatment often involves antibiotics, pain relief, and continued milk removal for breastfeeding mothers.
- Prevention strategies include proper breastfeeding techniques and addressing blocked ducts promptly.
What is Mastitis?
Mastitis refers to an inflammation of the breast tissue, which can be accompanied by an infection. This condition most commonly affects women who are breastfeeding, known as lactational mastitis, but it can also occur in non-lactating women and, rarely, in men. The inflammation can lead to pain, swelling, warmth, and redness of the breast. When an infection is present, it is typically bacterial, often caused by bacteria entering the breast through a cracked nipple. Understanding what is Mastitis is crucial for timely diagnosis and effective management, preventing potential complications such as a breast abscess.
Mastitis Symptoms and Causes
Recognizing mastitis symptoms and causes is vital for early intervention. The symptoms of mastitis can develop rapidly and may include:
- Breast pain or tenderness, often localized to one area
- Swelling of the breast
- A feeling of warmth in the affected breast
- Redness, often in a wedge-shaped pattern
- Fever (101°F or 38.3°C or greater)
- Chills
- Body aches
- Fatigue
The primary cause of mastitis is milk stasis, which occurs when milk is not adequately removed from the breast. This can lead to blocked milk ducts, creating an environment where bacteria can multiply. Bacteria, often from the skin’s surface or the infant’s mouth, can enter the milk ducts through cracks or breaks in the nipple. Risk factors for developing mastitis include sore or cracked nipples, wearing a tight bra, infrequent feedings, or a sudden decrease in feeding frequency. According to the Centers for Disease Control and Prevention (CDC), mastitis affects approximately 2-3% of breastfeeding women, though some studies report higher incidences.
Treating and Preventing Mastitis
Effective strategies for how to treat mastitis typically involve a combination of medical intervention and self-care. If a bacterial infection is suspected, a healthcare provider will usually prescribe antibiotics, which must be taken for the full course, even if symptoms improve quickly. Pain relievers, such as ibuprofen, can help manage pain and reduce inflammation. For breastfeeding mothers, it is generally recommended to continue breastfeeding or pumping from the affected breast to ensure complete milk removal, which helps clear blocked ducts and reduce milk stasis. Applying warm compresses and gentle massage to the affected area can also provide relief.
Alongside treatment, implementing mastitis prevention tips can significantly reduce the risk of recurrence. These tips focus on maintaining good breastfeeding practices and addressing potential issues promptly. Key prevention strategies include:
- Ensuring proper latch and positioning during breastfeeding to facilitate effective milk removal.
- Feeding frequently and on demand to prevent engorgement and milk stasis.
- Completely emptying one breast before offering the other.
- Avoiding tight bras or clothing that can restrict milk flow.
- Treating sore or cracked nipples promptly to prevent bacterial entry.
- Gradually weaning when discontinuing breastfeeding to avoid sudden milk buildup.
By understanding the condition, recognizing its symptoms, and adhering to both treatment and prevention guidelines, individuals can effectively manage and avoid mastitis.