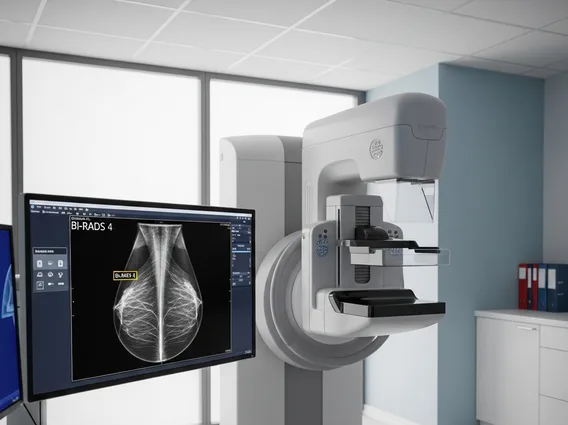
Mammography
Mammography is a specialized medical imaging technique that uses low-dose X-rays to examine breast tissue. It plays a crucial role in the early detection and diagnosis of breast diseases, including cancer.
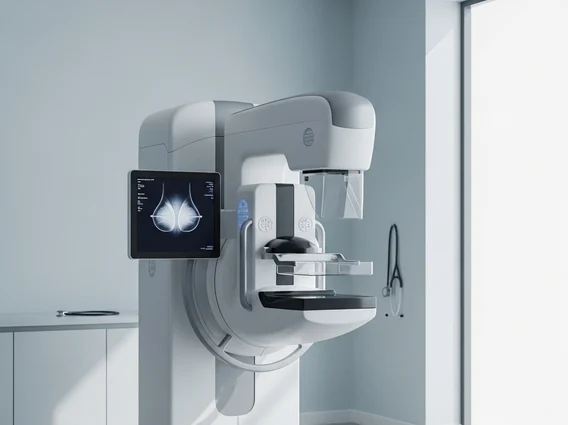
Key Takeaways
- Mammography is an X-ray imaging method used to screen for and diagnose breast conditions.
- It works by compressing the breast to spread tissue and reduce radiation dose, capturing detailed images.
- There are different types, including 2D (standard) and 3D (tomosynthesis), each offering unique advantages.
- Regular screening significantly improves the chances of early breast cancer detection, leading to better treatment outcomes.
- While highly beneficial, it involves minimal radiation exposure and has potential risks like false positives or negatives.
What is Mammography and How Does It Work?
Mammography is a medical imaging procedure that uses a low-dose X-ray system to create detailed images of the breast. These images, called mammograms, are used to look for changes in breast tissue that might not be felt during a physical exam. The primary goal is to detect breast cancer at its earliest, most treatable stages, often before symptoms develop.
The process of a mammogram involves positioning the breast between two plates on an X-ray machine. These plates gently compress the breast for a few seconds. Compression is essential because it helps to spread out the breast tissue, allowing for a clearer image, reducing the amount of radiation needed, and holding the breast still to prevent blurring. The X-rays then pass through the breast, and a detector captures the images, which are then reviewed by a radiologist to identify any abnormalities such as masses, calcifications, or distortions in the tissue.
Types of Mammography and Screening Recommendations
There are several different types of mammography explained, each with specific applications. The most common types include:
- 2D Mammography (Standard Digital Mammography): This traditional method captures two images of each breast (top-to-bottom and side-to-side). It is widely used for routine screening.
- 3D Mammography (Digital Breast Tomosynthesis – DBT): This advanced technique takes multiple X-ray images from different angles around the breast, which are then reconstructed into a 3D image. This allows radiologists to view breast tissue in thin layers, reducing the impact of overlapping tissue and potentially improving cancer detection, especially in dense breasts.
- Diagnostic Mammography: Used when a woman has breast symptoms (e.g., a lump, pain, nipple discharge) or when a screening mammogram shows an area of concern. It often involves more images and specialized views.
Understanding mammography guidelines and recommendations is crucial for effective breast health. Major health organizations provide guidance on when and how often women should undergo screening. For instance, the American Cancer Society (ACS) recommends annual mammograms for women starting at age 40 and continuing as long as they are in good health. The U.S. Preventive Services Task Force (USPSTF) recommends biennial screening for women aged 40 to 74. Individual recommendations may vary based on personal risk factors, such as a family history of breast cancer or genetic predispositions, which should be discussed with a healthcare provider. Regular screening is a cornerstone of early detection strategies.
Benefits and Risks of Mammogram Screening
The benefits and risks of mammogram screening are important considerations for individuals and healthcare providers. The primary benefit of regular mammography is its ability to detect breast cancer at an early stage, often before it can be felt. Early detection significantly increases the chances of successful treatment and improves survival rates. According to the Centers for Disease Control and Prevention (CDC), finding breast cancer early, when it’s small and has not spread, means there are more treatment options and a better chance of a full recovery.
However, like any medical procedure, mammography carries some risks. One concern is exposure to radiation. While the radiation dose from a mammogram is very low and considered safe, it is a factor to consider. Another potential risk is the possibility of false positives, where a mammogram indicates an abnormality that turns out not to be cancer, leading to anxiety and additional tests like biopsies. Conversely, false negatives can occur, meaning a mammogram appears normal even when cancer is present, which can delay diagnosis. Overdiagnosis, the detection of cancers that would never have caused harm during a woman’s lifetime, is also a debated risk. Despite these considerations, for most women, the benefits of early cancer detection through screening mammography far outweigh the potential risks.