Sebaceoma
Sebaceoma is a rare, benign skin tumor that originates from the sebaceous glands, which are responsible for producing oil (sebum) in the skin. While generally harmless, understanding this condition is important for proper diagnosis and management.
Key Takeaways
- Sebaceoma is a benign (non-cancerous) tumor derived from sebaceous glands, typically appearing on the face or scalp.
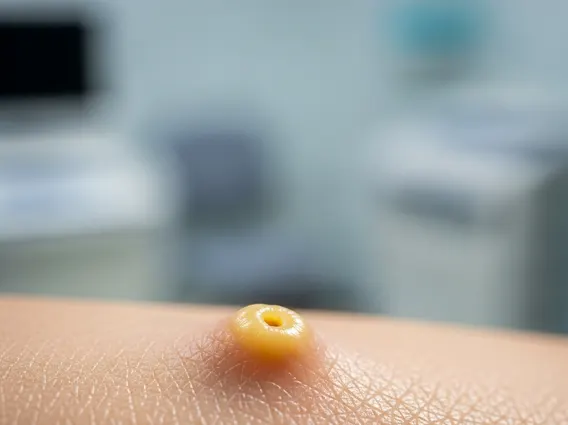
- It usually presents as a small, yellowish or flesh-colored papule or nodule and is often asymptomatic.
- Diagnosis relies primarily on a skin biopsy and histopathological examination to differentiate it from other skin lesions.
- While generally harmless, it can sometimes be associated with Muir-Torre syndrome, a genetic condition.
- Treatment often involves surgical excision, especially for cosmetic concerns or diagnostic confirmation.
What is Sebaceoma?
Sebaceoma refers to a rare, benign adnexal tumor of the skin that shows differentiation towards sebaceous glands. These tumors typically manifest as small, solitary, yellowish-to-flesh-colored papules or nodules, most commonly found on the head and neck, particularly the face and scalp. They are generally slow-growing and do not cause pain or discomfort, making them often unnoticed until they reach a noticeable size. As a type of sebaceoma skin condition information, it’s important to recognize that while benign, its presence warrants professional medical evaluation to rule out other conditions and confirm its nature.
Histologically, sebaceomas are characterized by a proliferation of mature and immature sebaceous cells, often arranged in lobules or cords within the dermis. Unlike sebaceous adenomas, sebaceomas typically show a more pronounced basaloid component, meaning they contain a higher proportion of undifferentiated cells resembling basal cells, alongside mature sebocytes. This distinction is crucial for pathologists in making an accurate diagnosis.
Sebaceoma Symptoms and Causes
The primary manifestation of sebaceoma is a visible skin lesion. The typical sebaceoma symptoms and causes are often subtle, as the tumor itself is usually asymptomatic. Key characteristics include:
- Appearance: A firm, well-defined papule or nodule, ranging from a few millimeters to several centimeters in diameter. Its color can vary from yellowish to skin-colored or slightly reddish.
- Location: Most frequently observed on the face, scalp, and neck, areas rich in sebaceous glands.
- Growth: Generally slow and non-invasive.
- Sensations: Typically painless and non-itchy, though occasional irritation may occur if the lesion is traumatized.
The exact cause of sebaceoma is often unknown, and most cases occur sporadically. However, there is a recognized association with Muir-Torre syndrome (MTS), a rare autosomal dominant hereditary cancer syndrome. MTS is characterized by the presence of at least one sebaceous tumor (such as sebaceoma, sebaceous adenoma, or sebaceous carcinoma) and at least one internal malignancy, most commonly colorectal cancer or genitourinary cancers. Therefore, individuals diagnosed with sebaceoma, especially if they have multiple lesions or a family history of certain cancers, may be screened for MTS.
Diagnosing Sebaceoma
The process of diagnosing sebaceoma typically begins with a clinical examination by a dermatologist. During this initial assessment, the doctor will inspect the lesion’s appearance, size, and location, and inquire about its duration and any associated symptoms. However, clinical presentation alone is often insufficient to definitively diagnose sebaceoma, as it can resemble other benign or even malignant skin lesions.
The definitive diagnosis of sebaceoma requires a skin biopsy, where a small tissue sample of the lesion is removed and sent to a pathology laboratory for microscopic examination. A dermatopathologist will analyze the tissue to identify the characteristic histological features of sebaceoma, such as the proliferation of sebaceous cells at various stages of maturation and the presence of basaloid cells. This detailed examination helps differentiate sebaceoma from other sebaceous neoplasms, such as sebaceous adenoma, sebaceous carcinoma, or basal cell carcinoma with sebaceous differentiation. Once diagnosed, treatment typically involves surgical excision, which is often curative and also serves to confirm the diagnosis.