Meningeal Leukemia
Meningeal Leukemia is a serious complication of various types of leukemia, characterized by the spread of cancer cells to the central nervous system. This condition requires specialized diagnostic and treatment approaches due to its unique challenges and potential impact on neurological function.

Key Takeaways
- Meningeal Leukemia involves the infiltration of leukemia cells into the cerebrospinal fluid and surrounding membranes of the brain and spinal cord.
- Symptoms often include neurological manifestations like headaches, vision changes, and seizures, necessitating prompt diagnosis.
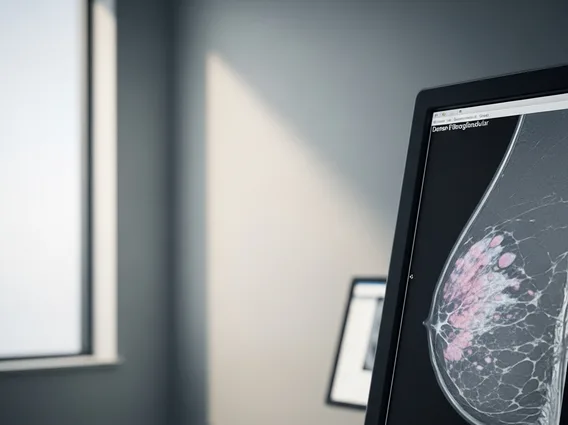
- Diagnosis relies on cerebrospinal fluid analysis and imaging studies to confirm the presence of leukemia cells.
- Treatment typically involves intrathecal chemotherapy and sometimes radiation therapy to target cancer cells in the CNS.
- Prognosis varies significantly depending on the underlying leukemia type, stage, and response to treatment.
What is Meningeal Leukemia?
Meningeal Leukemia refers to the presence of leukemia cells in the cerebrospinal fluid (CSF) and the meninges, which are the protective membranes surrounding the brain and spinal cord. This complication can arise from various types of leukemia, including acute lymphoblastic leukemia (ALL), acute myeloid leukemia (AML), and chronic leukemias, although it is more common in acute forms, especially ALL. The central nervous system (CNS) is considered a “sanctuary site” for leukemia cells because many systemic chemotherapy drugs cannot effectively cross the blood-brain barrier, allowing cancer cells to evade treatment and proliferate in this protected environment.
The development of meningeal leukemia can lead to significant neurological complications, impacting a patient’s quality of life and overall prognosis. While relatively rare compared to systemic leukemia, its occurrence underscores the importance of comprehensive treatment strategies that include CNS prophylaxis, particularly in high-risk leukemia types. According to oncology experts, effective management requires a deep understanding of the disease’s unique pathophysiology within the CNS.
Meningeal Leukemia Symptoms and Diagnosis
The presentation of meningeal leukemia symptoms can be varied and often reflects increased intracranial pressure or direct neurological impairment. Common symptoms may include persistent headaches, nausea, vomiting, vision changes (such as blurred or double vision), and dizziness. More severe manifestations can involve seizures, weakness or numbness in limbs, facial paralysis, difficulty with balance, or changes in mental status.
Diagnosing meningeal leukemia typically involves a combination of clinical evaluation, imaging, and laboratory tests. The primary diagnostic tool is a lumbar puncture (spinal tap) to collect cerebrospinal fluid (CSF) for analysis. The CSF is then examined under a microscope for the presence of leukemia cells. Other diagnostic procedures may include:
- CSF Cytology: Microscopic examination to identify malignant cells.
- Flow Cytometry: A more sensitive test that can detect leukemia cells even when they are present in low numbers.
- MRI of the Brain and Spine: Imaging studies can help identify signs of meningeal involvement, such as thickening of the meninges or hydrocephalus (excess fluid in the brain), though a normal MRI does not rule out the condition.
Early and accurate diagnosis is crucial for initiating timely treatment and preventing irreversible neurological damage.
Treatment Options and Prognosis for Meningeal Leukemia
Treatment for meningeal leukemia treatment options are specifically designed to deliver chemotherapy agents directly into the central nervous system, bypassing the blood-brain barrier. The primary approach is intrathecal chemotherapy, where anti-cancer drugs are injected directly into the CSF, usually through a lumbar puncture or a surgically implanted reservoir called an Ommaya reservoir. Common drugs used include methotrexate, cytarabine, and corticosteroids.
In some cases, radiation therapy to the brain and/or spinal cord may be used, either alone or in combination with intrathecal chemotherapy, especially for patients who do not respond well to chemotherapy or have extensive CNS involvement. The choice of treatment depends on the type of leukemia, the extent of CNS involvement, the patient’s age, and overall health. Systemic chemotherapy also continues to treat the underlying leukemia, but its CNS penetration is limited.
The meningeal leukemia prognosis varies significantly and is influenced by several factors, including the type of underlying leukemia, the patient’s age, the extent of CNS involvement at diagnosis, and the response to treatment. While meningeal leukemia is a serious complication, advancements in diagnostic techniques and treatment strategies have improved outcomes for many patients. Continuous monitoring through regular lumbar punctures is often necessary to assess treatment effectiveness and detect any recurrence. Long-term management focuses on preventing relapse and managing any residual neurological deficits.