Guillain Barre Syndrome
Guillain Barre Syndrome (GBS) is a rare and serious autoimmune disorder that affects the peripheral nervous system. It is characterized by the body’s immune system mistakenly attacking its own nerve cells, leading to muscle weakness and, in severe cases, paralysis.

Key Takeaways
- Guillain Barre Syndrome (GBS) is a rare autoimmune disorder where the immune system attacks peripheral nerves.
- It often follows an infection, leading to rapid onset of muscle weakness and tingling sensations.
- Symptoms can range from mild weakness to severe paralysis, potentially affecting breathing and requiring intensive care.
- Diagnosis involves clinical examination, nerve conduction studies, and spinal fluid analysis.
- Treatment focuses on reducing the severity of the illness and accelerating recovery through therapies like intravenous immunoglobulin (IVIg) or plasma exchange.
What is Guillain Barre Syndrome (GBS)?
Guillain Barre Syndrome (GBS) is a rare neurological disorder in which the body’s immune system attacks the myelin sheath, the protective covering around peripheral nerves, or the nerves themselves. This damage disrupts the signals between the brain and the rest of the body, leading to muscle weakness, numbness, and sometimes paralysis. The condition can affect anyone, regardless of age or gender, though it is slightly more common in adults and males. According to the Centers for Disease Control and Prevention (CDC), GBS affects approximately 3,000 to 6,000 people in the United States each year, making it a relatively uncommon but significant health concern.
The onset of GBS is typically sudden, with symptoms often progressing rapidly over days or weeks. While most individuals recover fully or with minor residual weakness, some may experience long-term neurological issues. Early recognition and medical intervention are crucial for managing the condition and improving outcomes.
Guillain Barre Syndrome Symptoms and Causes
The presentation of Guillain Barre Syndrome symptoms usually begins with weakness and tingling sensations in the legs, which can then spread to the arms and upper body. These symptoms are often symmetrical, affecting both sides of the body equally. The severity of symptoms can vary widely among individuals, from mild weakness to complete paralysis.
Common symptoms include:
- Progressive muscle weakness, often starting in the legs and ascending.
- Tingling, prickling, or numbness in the fingers, toes, ankles, or wrists.
- Unsteady walking or inability to walk or climb stairs.
- Severe pain that may feel achy or cramp-like and may worsen at night.
- Difficulty with eye movement, facial movements, speaking, chewing, or swallowing.
- Severe fatigue.
- Rapid heart rate.
- Low or high blood pressure.
- Difficulty with bladder control or bowel function.
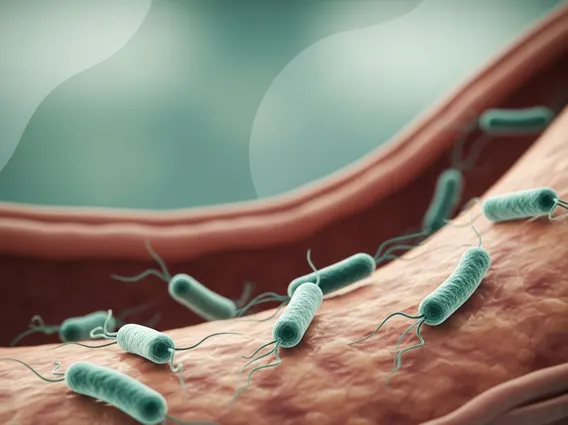
The exact Guillain Barre Syndrome causes are not fully understood, but it is widely accepted as an autoimmune response. In most cases, GBS is triggered by an acute infection, such as a viral or bacterial illness. Common triggers include infections with Campylobacter jejuni (a common cause of food poisoning), influenza virus, Zika virus, cytomegalovirus (CMV), and Epstein-Barr virus (EBV). Less commonly, surgery or vaccinations have been associated with GBS, though the link is rare and the benefits of vaccination far outweigh the minimal risk.
Diagnosing and Treating Guillain Barre Syndrome
Diagnosing Guillain Barre Syndrome requires a thorough clinical evaluation, as its symptoms can mimic those of other neurological disorders. A doctor will typically perform a neurological examination, assessing muscle strength, reflexes, and sensory responses. Key diagnostic tests include a lumbar puncture (spinal tap) to analyze cerebrospinal fluid for elevated protein levels without an increase in white blood cells, which is characteristic of GBS. Additionally, nerve conduction studies and electromyography (NCS/EMG) are used to measure the speed of nerve signal transmission and assess muscle electrical activity, helping to identify nerve damage.
While there is no cure for GBS, Guillain Barre Syndrome treatment options aim to reduce the severity of the illness, accelerate recovery, and manage complications. The primary treatments involve therapies that modify the immune system’s attack on the nerves:
| Treatment Option | Mechanism |
|---|---|
| Intravenous Immunoglobulin (IVIg) | Involves infusing healthy antibodies into the bloodstream to block the harmful antibodies that attack nerves. |
| Plasma Exchange (Plasmapheresis) | A procedure that removes the liquid part of the blood (plasma) and separates it from blood cells, removing harmful antibodies before returning the blood cells to the body. |
These treatments are most effective when administered early in the disease course. Supportive care is also critical, especially for patients with severe symptoms. This may include mechanical ventilation if breathing muscles are affected, pain management, and physical and occupational therapy to help regain strength and function during recovery. Recovery from GBS can be a long process, ranging from weeks to several years, and some individuals may experience residual weakness or fatigue.