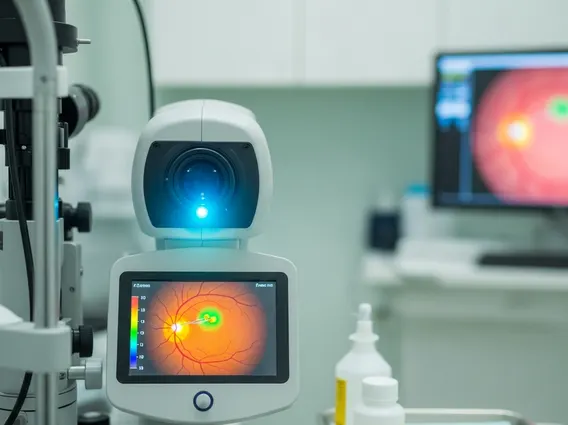
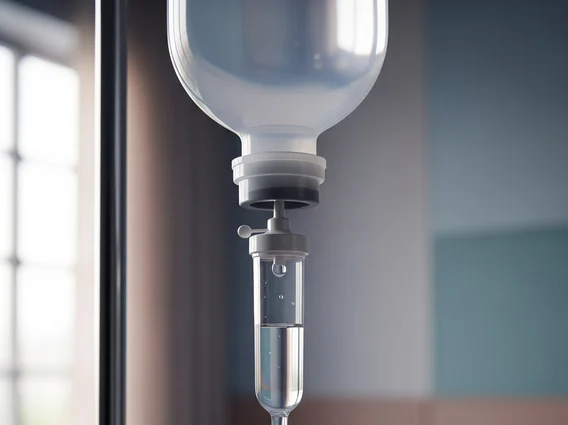
Fluid Replacement Therapy
Fluid Replacement Therapy is a critical medical intervention designed to restore and maintain the body’s fluid and electrolyte balance. It plays a vital role in managing various conditions, from acute dehydration to significant blood loss, ensuring optimal physiological function.
Key Takeaways
- Fluid Replacement Therapy is essential for correcting fluid and electrolyte imbalances in the body.
- It encompasses various methods, including oral rehydration solutions and intravenous fluids like crystalloids and colloids.
- The primary benefits include preventing dehydration, supporting organ function, and aiding recovery from illness or injury.
- Effective therapy requires adherence to specific guidelines tailored to the patient’s condition, age, and type of fluid loss.
- Medical supervision is crucial to ensure safe and appropriate fluid administration.
What is Fluid Replacement Therapy?
Fluid Replacement Therapy refers to the medical practice of replenishing lost bodily fluids and electrolytes to maintain physiological homeostasis. This intervention is crucial in situations where the body loses fluids faster than it can replace them, such as severe dehydration, hemorrhage, burns, or during and after surgical procedures. The goal is to restore circulating blood volume, correct electrolyte imbalances, and support organ perfusion, which is vital for preventing complications and promoting recovery. Without adequate fluid replacement, conditions like hypovolemic shock, kidney failure, and other severe systemic dysfunctions can occur.
Types and Benefits of Fluid Replacement Therapy
The approach to fluid replacement varies depending on the patient’s condition, the severity of fluid loss, and the specific electrolytes that need replenishment. The primary types of fluid replacement therapy include oral rehydration and intravenous (IV) administration.
- Oral Rehydration Solutions (ORS): These are typically used for mild to moderate dehydration, especially in cases of gastroenteritis. ORS contain a balanced mixture of salts and sugars that facilitate water absorption in the intestines. The World Health Organization (WHO) estimates that ORS can prevent up to 93% of deaths from diarrheal dehydration in children, highlighting its effectiveness and accessibility.
- Intravenous (IV) Fluids: For more severe dehydration, significant blood loss, or when oral intake is not possible, IV fluids are administered directly into the bloodstream. These are broadly categorized into:
- Crystalloids: Solutions containing small molecules that can easily pass from the bloodstream into tissues. Examples include normal saline (0.9% sodium chloride) and Ringer’s lactate, commonly used for general fluid resuscitation.
- Colloids: Solutions containing larger molecules that tend to remain in the bloodstream, effectively increasing intravascular volume. Examples include albumin and synthetic starches, often used in cases of significant blood loss or severe hypovolemia.
The benefits of fluid replacement therapy are extensive and critical for patient well-being. It prevents and treats dehydration, which can impair organ function and lead to serious health issues. By maintaining adequate blood volume and electrolyte balance, it supports cardiovascular stability, ensures proper kidney function, and facilitates nutrient and oxygen delivery to tissues. This therapy is instrumental in accelerating recovery from various illnesses, injuries, and surgical procedures, significantly improving patient outcomes.
Guidelines for Fluid Replacement Therapy
Effective fluid replacement therapy guidelines are essential for safe and appropriate treatment. These guidelines are developed based on extensive medical research and clinical experience, taking into account various factors unique to each patient. Key considerations include the patient’s age, body weight, underlying medical conditions (e.g., heart failure, kidney disease), the type and severity of fluid loss, and electrolyte status.
Healthcare professionals carefully assess these factors to determine the appropriate type, volume, and rate of fluid administration. For instance, children and the elderly often require different fluid management strategies due to variations in body composition and organ function. Monitoring the patient’s response, including urine output, blood pressure, heart rate, and electrolyte levels, is continuous to adjust the therapy as needed. Adherence to these guidelines minimizes risks such as fluid overload, electrolyte imbalances, and other potential complications, ensuring that the therapy is both effective and safe for the patient.