False Positive Test Result
A False Positive Test Result can be a source of significant anxiety and confusion for patients, indicating the presence of a condition when it is not actually there. Understanding the nature of these results is crucial for proper medical interpretation and subsequent management.

Key Takeaways
- A False Positive Test Result indicates a condition or disease when it is not truly present.
- These results can stem from various factors, including test sensitivity, technical errors, and biological variations.
- False positives often necessitate further diagnostic testing to confirm or rule out a diagnosis.
- Effective communication with healthcare providers is essential for interpreting and managing such results.
- While concerning, a false positive does not mean a definitive diagnosis and often leads to reassurance after follow-up.
What is a False Positive Test Result?
A False Positive Test Result occurs when a medical test indicates that a person has a specific disease or condition, but in reality, they do not. This outcome can be particularly distressing, as it suggests a health problem that is not present, leading to unnecessary worry and potentially further invasive or costly diagnostic procedures. These results are distinct from true positives (correctly identifying a condition), true negatives (correctly identifying the absence of a condition), and false negatives (failing to identify a condition that is present).
The occurrence of a false positive is often related to the inherent limitations of diagnostic tests, which are designed to balance sensitivity (the ability to correctly identify those with the disease) and specificity (the ability to correctly identify those without the disease). No test is 100% perfect, and a certain rate of false positives is often an accepted trade-off, especially in screening tests designed to catch as many potential cases as possible, even if it means some healthy individuals are flagged.
Causes of False Positive Test Results
Several factors can contribute to the occurrence of a False Positive Test Result. These causes can range from technical issues in the laboratory to biological variations within individuals. Recognizing these underlying reasons is vital for healthcare professionals when evaluating test outcomes.
- Test Sensitivity and Specificity: Tests with high sensitivity might produce more false positives to ensure no true cases are missed. Conversely, tests with very high specificity are less likely to yield false positives but might miss some true cases.
- Cross-Reactivity: Some tests detect markers that are similar to, but not identical with, the target substance. Other substances or conditions in the body can mimic the presence of the disease marker, leading to a false positive.
- Technical or Human Error: Mistakes during sample collection, handling, processing, or interpretation in the laboratory can lead to inaccurate results.
- Biological Variations: Factors such as pregnancy, certain medications, benign conditions, or even recent infections can temporarily alter biological markers, causing a test to register positive when no serious disease is present. For example, elevated prostate-specific antigen (PSA) levels, often used to screen for prostate cancer, can also be caused by benign prostatic hyperplasia or inflammation, leading to a false positive result in about 75% of men with elevated PSA who undergo biopsy, according to the American Cancer Society.
An accurate understanding false positive medical tests requires considering these various contributing factors, as they help explain why an initial positive result may not always indicate a definitive diagnosis.
Interpreting and Managing False Positive Results
When faced with a False Positive Test Result, the immediate priority is to avoid panic and engage in clear communication with healthcare providers. The process of interpreting and managing these results typically involves further investigation to confirm or rule out the initial finding.
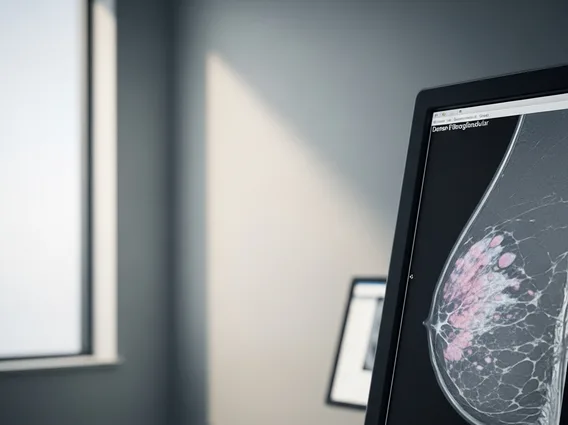
The first step in managing a false positive is often a confirmatory test. This might involve repeating the initial test, performing a different type of test that is more specific, or conducting more invasive diagnostic procedures such as biopsies or imaging scans. For instance, if a screening mammogram shows a suspicious area, a follow-up diagnostic mammogram, ultrasound, or MRI is usually recommended before any definitive conclusions are drawn. According to the Centers for Disease Control and Prevention (CDC), about 1 in 10 women who get a mammogram will be called back for more tests, but most of these follow-ups will not lead to a cancer diagnosis.
Healthcare providers play a crucial role in explaining the implications of a false positive, detailing the next steps, and alleviating patient anxiety. It is important for patients to ask questions, understand the likelihood of a true positive versus a false positive, and participate in shared decision-making regarding further diagnostic pathways. Ultimately, while initially concerning, a false positive result often serves as a trigger for a more thorough evaluation that eventually provides reassurance and prevents unnecessary treatment.