Extraskeletal Myxoid Chondrosarcoma
Extraskeletal Myxoid Chondrosarcoma is a rare and distinct type of soft tissue sarcoma, characterized by its unique cellular features and tendency to arise outside of bone. Understanding this condition is crucial for accurate diagnosis and effective management.

Key Takeaways
- Extraskeletal Myxoid Chondrosarcoma (EMC) is a rare soft tissue cancer that develops outside of bone.
- It typically presents as a slow-growing, painless mass, most often in the extremities.
- Diagnosis relies on imaging studies and a definitive biopsy with histopathological and molecular analysis.
- The primary treatment is surgical removal, sometimes supplemented with radiation therapy.
- While generally slow-growing, EMC has a risk of late recurrence and metastasis, necessitating long-term follow-up.
What is Extraskeletal Myxoid Chondrosarcoma?
Extraskeletal Myxoid Chondrosarcoma (EMC) is a malignant tumor originating from soft tissues, rather than bone, which is characteristic of most chondrosarcomas. It is a rare form of sarcoma, accounting for less than 3% of all soft tissue sarcomas. This tumor is distinguished by its myxoid (gelatinous) matrix and cells that show features of cartilage differentiation. EMC most commonly develops in the deep soft tissues of the extremities, particularly the thighs and buttocks, but can also occur in the trunk, head, and neck regions. Its exact cause is unknown, but it is often associated with specific chromosomal translocations, particularly those involving the NR4A3 gene.
Unlike conventional chondrosarcomas that arise from cartilage within bones, EMC is truly “extraskeletal,” meaning it forms in tissues like muscle, fat, or connective tissue. It typically affects adults, with a slight male predominance, and is usually found in individuals between 30 and 70 years old. The slow-growing nature of this tumor often means it can reach a considerable size before being detected, making early recognition challenging.
Symptoms and Diagnosis of Extraskeletal Myxoid Chondrosarcoma
The most common of the extraskeletal myxoid chondrosarcoma symptoms is the presence of a slow-growing, often painless, soft tissue mass. This mass can be palpable and may gradually increase in size over months or even years. Depending on its location, it might cause discomfort or functional impairment if it presses on nerves, blood vessels, or joints. Less frequently, patients may experience localized pain or swelling, especially if the tumor grows rapidly or is situated in a sensitive area.
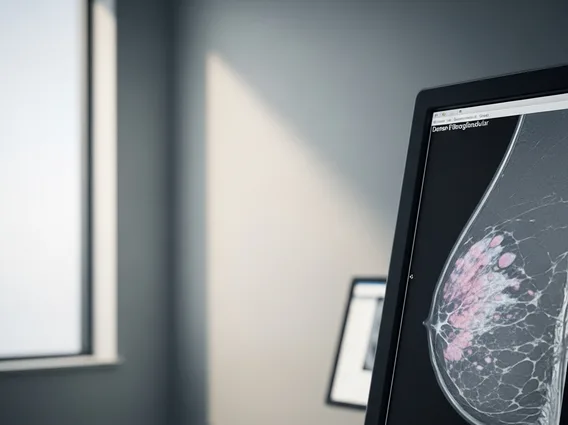
Diagnosing EMC typically involves a combination of imaging studies and a tissue biopsy. Initial evaluation often includes magnetic resonance imaging (MRI) or computed tomography (CT) scans to assess the tumor’s size, exact location, and its relationship to surrounding structures. These imaging modalities can help differentiate EMC from other soft tissue masses. However, a definitive diagnosis requires a biopsy, where a tissue sample is taken and examined under a microscope by a pathologist. Histopathological analysis reveals characteristic features such as a lobulated growth pattern, abundant myxoid matrix, and cords or nests of uniform, small chondroblast-like cells. Immunohistochemistry and molecular genetic testing, looking for specific translocations like t(9;22)(q22;q12) involving the EWSR1 and NR4A3 genes, are crucial for confirming the diagnosis and distinguishing EMC from other myxoid tumors.
Common diagnostic steps include:
- Physical Examination: To identify and characterize the palpable mass.
- Imaging Studies: MRI is preferred for soft tissue evaluation; CT scans are useful for assessing distant metastasis.
- Biopsy: Incisional or core needle biopsy for tissue acquisition.
- Histopathology: Microscopic examination of the tissue sample.
- Molecular Testing: Genetic analysis to confirm specific translocations.
Treatment and Prognosis for Extraskeletal Myxoid Chondrosarcoma
The primary extraskeletal myxoid chondrosarcoma treatment is surgical resection with wide, clear margins. Achieving complete surgical removal is critical for local control and improving patient outcomes. Due to the tumor’s often infiltrative nature and proximity to vital structures, obtaining clear margins can sometimes be challenging. In cases where complete resection is difficult or margins are positive, adjuvant radiation therapy may be considered to reduce the risk of local recurrence. The role of chemotherapy in EMC is less well-defined compared to other sarcomas, as these tumors tend to be less responsive to conventional cytotoxic agents. Targeted therapies are being explored, particularly for advanced or metastatic disease, given the specific genetic alterations associated with EMC.
The extraskeletal myxoid chondrosarcoma prognosis is generally considered to be more favorable than many other high-grade sarcomas, largely due to its typically indolent (slow-growing) nature. However, EMC is known for its potential for late local recurrences and distant metastases, which can occur many years after initial treatment. Metastases most commonly spread to the lungs, bone, and lymph nodes. Factors influencing prognosis include tumor size, location, the completeness of surgical resection, and the presence of metastasis at diagnosis. Regular, long-term follow-up with imaging is essential for patients with EMC to monitor for recurrence or metastasis, allowing for timely intervention if needed. According to a study published in the journal Cancer, the 5-year overall survival rate for EMC patients is approximately 80-90%, but this can decrease significantly with metastatic disease.