Calcium Infusion Test
The Calcium Infusion Test is a specialized diagnostic procedure used in medicine to assess how the body regulates calcium levels. It provides crucial insights into various endocrine and metabolic conditions affecting calcium homeostasis.
Key Takeaways
- The Calcium Infusion Test evaluates the body’s calcium regulation mechanisms.
- It helps diagnose conditions affecting parathyroid glands and bone metabolism.
- The test involves intravenous administration of calcium and subsequent blood sampling.
- Results are interpreted based on changes in calcium, parathyroid hormone (PTH), and other markers.
- It is a valuable tool for understanding complex calcium disorders.
What is a Calcium Infusion Test and Its Purpose?
A Calcium Infusion Test refers to a diagnostic procedure designed to evaluate the body’s ability to maintain calcium homeostasis. This test involves the controlled intravenous administration of calcium while monitoring the body’s response, particularly changes in blood calcium and parathyroid hormone (PTH) levels. It is primarily used to investigate disorders related to calcium metabolism, which can impact bone health, nerve function, and muscle contraction.
The purpose of calcium infusion test is multifaceted. It helps clinicians differentiate between various causes of abnormal calcium levels, such as hyperparathyroidism (overactive parathyroid glands) or hypoparathyroidism (underactive parathyroid glands), and other conditions like familial hypocalciuric hypercalcemia (FHH). By observing how the body reacts to an influx of calcium, medical professionals can gain a clearer understanding of the underlying mechanisms regulating calcium, aiding in accurate diagnosis and appropriate treatment planning. For instance, in cases of suspected primary hyperparathyroidism, the test can help confirm the diagnosis by showing an inappropriate PTH response to elevated calcium.
Performing the Calcium Infusion Test
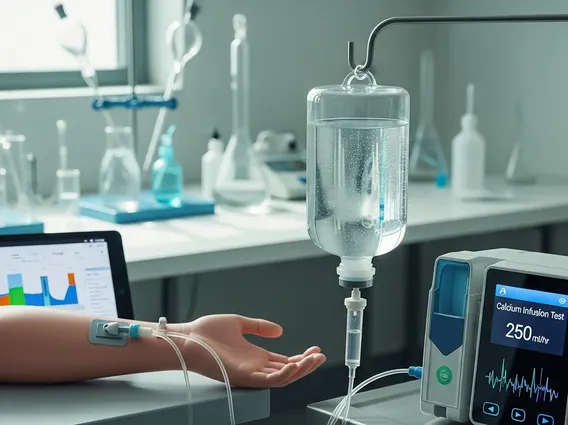
Performing the Calcium Infusion Test involves a specific protocol to ensure accurate results. Typically, the patient is required to fast for a certain period before the test. The general steps involved are:
- Baseline Blood Draw: Initial blood samples are collected to measure calcium, parathyroid hormone (PTH), and sometimes other relevant markers.
- Calcium Infusion: A controlled dose of calcium (e.g., calcium gluconate) is administered intravenously over a specified duration, often several hours.
- Serial Blood Samples: Multiple blood samples are drawn at predetermined intervals during and after the infusion to track changes in calcium and PTH levels.
- Monitoring: Patients are continuously monitored for any potential adverse reactions throughout the procedure.
The exact timing and number of blood draws can vary based on the specific diagnostic question and the protocol of the testing facility. The entire procedure typically takes several hours, and patients may be advised to avoid certain medications or supplements prior to the test that could interfere with calcium metabolism.
Interpreting Calcium Infusion Test Results
Calcium infusion test results interpretation requires a thorough understanding of calcium and parathyroid hormone physiology. The results are analyzed by comparing the changes in calcium and PTH levels from baseline throughout the infusion period. In a healthy individual, an increase in blood calcium due to the infusion would typically lead to a suppression of PTH secretion by the parathyroid glands, as the body attempts to restore calcium balance.
However, in conditions like primary hyperparathyroidism, the parathyroid glands may not adequately suppress PTH in response to the elevated calcium, indicating autonomous hormone production. Conversely, in familial hypocalciuric hypercalcemia (FHH), the body’s calcium-sensing receptors are less sensitive, leading to higher calcium levels without appropriate PTH suppression, but with distinct urinary calcium excretion patterns that help differentiate it from primary hyperparathyroidism. The specific patterns of calcium and PTH response help clinicians pinpoint the exact nature of the calcium dysregulation. For example, a study published in the Journal of Clinical Endocrinology & Metabolism highlighted the test’s utility in distinguishing between these conditions, which is crucial for guiding surgical versus non-surgical management.