Interleukin 5
Interleukin 5 (IL-5) is a crucial cytokine that plays a central role in the immune system, primarily by regulating the growth, differentiation, and activation of eosinophils. Understanding IL-5 is vital for comprehending various inflammatory and allergic conditions.
Key Takeaways
- Interleukin 5 (IL-5) is a cytokine produced by immune cells, primarily T-helper 2 cells.
- Its main function is to promote the development, survival, and activation of eosinophils.
- IL-5 exerts its effects by binding to specific receptors on eosinophil surfaces.
- Elevated IL-5 levels are a key driver of inflammation in severe eosinophilic asthma and other eosinophilic diseases.
- Targeting IL-5 or its receptor is a therapeutic strategy for these conditions.
What is Interleukin 5 (IL-5)?
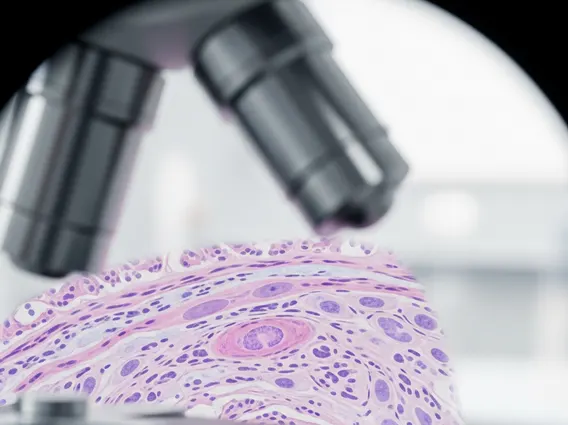
Interleukin 5 (IL-5) is a type of signaling protein, known as a cytokine, belonging to the hematopoietic growth factor family. It is predominantly produced by T-helper 2 (Th2) lymphocytes, but also by other immune cells such as mast cells, eosinophils, and innate lymphoid cells type 2 (ILC2s). IL-5 is a homodimeric glycoprotein, meaning it consists of two identical protein subunits. Its primary biological function revolves around the regulation of eosinophils, a type of white blood cell involved in allergic reactions and defense against parasites. The presence and activity of IL-5 are critical for the body’s immune response, particularly in contexts involving allergic inflammation.
Interleukin 5 Function and Mechanism of Action
The core interleukin 5 function is to orchestrate the lifecycle and activity of eosinophils. IL-5 promotes the proliferation of eosinophil precursors in the bone marrow, their differentiation into mature eosinophils, and their release into the bloodstream. Once in circulation, IL-5 facilitates the recruitment of eosinophils to sites of inflammation and enhances their survival by inhibiting programmed cell death (apoptosis). This sustained presence and activation of eosinophils are central to their role in immune responses, both beneficial and detrimental.
The interleukin 5 mechanism of action involves its binding to a specific receptor, the IL-5 receptor (IL-5R), found on the surface of eosinophils and their progenitor cells. The IL-5R is composed of an alpha subunit (IL-5Rα), which is specific for IL-5, and a common beta subunit (βc), which is shared with the receptors for IL-3 and GM-CSF. Upon IL-5 binding, the receptor subunits dimerize, triggering intracellular signaling cascades, primarily through the Janus kinase (JAK) and signal transducer and activator of transcription (STAT) pathways. These pathways lead to gene expression changes that promote eosinophil growth, differentiation, activation, and prolonged survival. This intricate signaling ensures that eosinophils are effectively mobilized and maintained where they are needed.
Interleukin 5’s Role in Asthma and Eosinophilic Diseases
The heightened activity of IL-5 is a significant driver in several inflammatory conditions, most notably severe eosinophilic asthma. In this form of asthma, elevated levels of IL-5 lead to an overproduction and accumulation of eosinophils in the airways. These activated eosinophils release various inflammatory mediators, including cytotoxic proteins, cytokines, and lipid mediators, which contribute to airway inflammation, bronchoconstriction, mucus hypersecretion, and airway remodeling. This chronic inflammation results in persistent asthma symptoms, frequent exacerbations, and reduced lung function. According to the American Lung Association, eosinophilic asthma accounts for approximately 50% of severe asthma cases, highlighting the clinical relevance of IL-5 in this patient population.
Beyond asthma, interleukin 5’s role in asthma extends to other eosinophilic diseases, where it similarly drives pathology. These conditions include hypereosinophilic syndrome, eosinophilic esophagitis, and certain drug reactions. In these disorders, uncontrolled eosinophil activation, often mediated by IL-5, can lead to tissue damage and organ dysfunction. The understanding of IL-5’s critical involvement has led to the development of targeted therapies, such as monoclonal antibodies that block IL-5 or its receptor, offering significant therapeutic benefits for patients with severe eosinophilic conditions by reducing eosinophil counts and mitigating inflammation.