Spinal Block
A spinal block is a common regional anesthesia technique used to numb specific areas of the body for surgical procedures or pain management. It offers an effective alternative to general anesthesia in many clinical scenarios.
Key Takeaways
- A spinal block is a regional anesthetic injected into the cerebrospinal fluid surrounding the spinal cord.
- It temporarily blocks nerve signals, providing numbness and muscle relaxation below the injection site.
- Commonly used for lower body surgeries, C-sections, and certain orthopedic procedures.
- Benefits include faster recovery, reduced opioid use, and avoidance of general anesthesia risks.
- Potential side effects range from headache and low blood pressure to rare neurological complications.
What is Spinal Block?
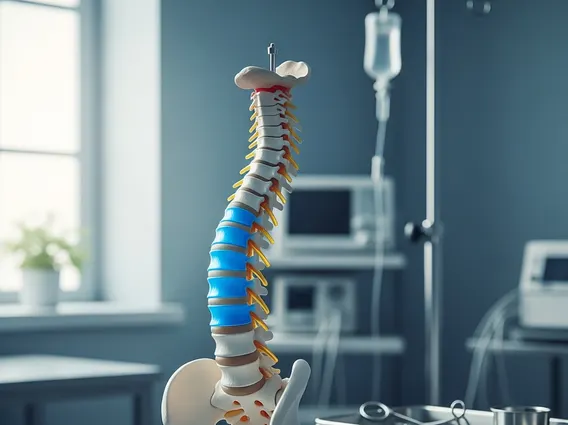
Spinal Block is a form of regional anesthesia that involves injecting a local anesthetic into the cerebrospinal fluid (CSF) in the subarachnoid space surrounding the spinal cord. This procedure temporarily blocks nerve impulses from the spinal nerves, resulting in numbness and muscle relaxation in the lower part of the body. It is often chosen for surgeries below the waist, providing effective pain relief and allowing the patient to remain awake during the procedure.
The spinal block procedure typically involves the patient sitting or lying on their side, with their back curved to widen the spaces between the vertebrae. After sterilizing the skin and numbing the injection site with a local anesthetic, a thin needle is carefully inserted into the subarachnoid space, usually between the lumbar vertebrae. Once the needle is correctly positioned, the anesthetic medication is injected, and its effects usually begin within minutes, lasting for several hours depending on the specific medication and dosage used. This technique is distinct from an epidural, where the anesthetic is injected into the epidural space, outside the dura mater.
How Spinal Block Anesthesia Works, Uses, and Benefits
How spinal block anesthesia works involves the direct delivery of anesthetic agents to the nerve roots as they exit the spinal cord. These medications prevent nerve cells from transmitting electrical signals, effectively blocking sensations of pain, touch, and temperature, as well as motor function, in the areas supplied by those nerves. The rapid onset and profound block make it highly effective for acute pain management during and after surgery.
The uses and benefits of spinal block are extensive, particularly in surgical settings. It is frequently employed for:
- Cesarean sections (C-sections)
- Hip and knee replacements
- Urological procedures
- Lower extremity vascular surgeries
- Hernia repairs
- Perineal and rectal surgeries
Benefits include a faster recovery profile compared to general anesthesia, reduced need for postoperative opioid pain medication, and a lower incidence of nausea and vomiting. Patients often experience less fatigue and can mobilize sooner. According to the World Health Organization (WHO), regional anesthesia techniques like spinal blocks can reduce the risk of certain postoperative complications, especially in elderly or high-risk patients.
Spinal Block Side Effects and Risks
While generally safe and effective, there are potential spinal block side effects and risks that patients should be aware of. Most side effects are temporary and manageable, but some rare complications can be more serious.
Common side effects include:
- Post-dural puncture headache (PDPH): This is a specific type of headache that can occur after the needle punctures the dura mater, allowing CSF to leak. It typically worsens when sitting or standing and improves when lying down.
- Hypotension (low blood pressure): Anesthetic agents can cause blood vessels to dilate, leading to a drop in blood pressure, which is usually managed with fluids and medication.
- Nausea and vomiting: Can occur due to low blood pressure or the effect of medication.
- Urinary retention: Temporary difficulty in passing urine.
- Back pain: Mild discomfort at the injection site.
More serious, though rare, risks include:
- Nerve damage: While extremely rare, direct needle trauma or hematoma formation can potentially cause temporary or permanent nerve injury.
- Infection: Introduction of bacteria into the spinal canal (meningitis or abscess).
- Hematoma: Blood clot formation around the spinal cord, which can compress nerves.
- Total spinal block: Spread of the anesthetic higher than intended, affecting breathing and heart function, requiring immediate medical intervention.
Healthcare providers take precautions to minimize these risks, including careful patient selection, sterile technique, and continuous monitoring during and after the procedure.