Side To End Coloanal Anastomosis
Side To End Coloanal Anastomosis is a specialized surgical procedure primarily used in the treatment of low rectal cancer. It aims to remove the diseased part of the rectum while preserving anal sphincter function, thereby maintaining bowel control and quality of life for patients.
Key Takeaways
- Side To End Coloanal Anastomosis is a complex surgical technique for treating low rectal cancer, focusing on sphincter preservation.
- The procedure involves the removal of the diseased rectum and the direct connection of the colon to the anus.
- Recovery typically includes a hospital stay, dietary adjustments, and a gradual return to normal activities, often with temporary bowel diversion.
- Success rates are generally high for achieving local cancer control and preserving functional bowel control.
- Potential challenges during recovery include changes in bowel habits and the risk of anastomotic complications.
What is Side To End Coloanal Anastomosis?
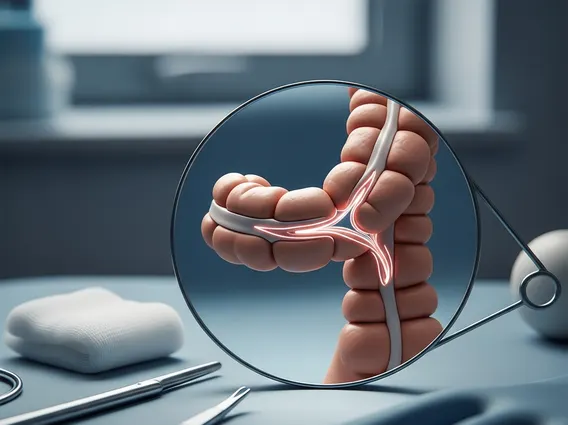
Side To End Coloanal Anastomosis refers to a surgical technique performed primarily for patients with low rectal cancer. This procedure involves the complete removal of the rectum (proctectomy) and then connecting the side of the remaining colon to the end of the anal canal. The goal is to excise the tumor completely while preserving the integrity of the anal sphincter muscles, which are crucial for maintaining continence. This approach allows for the restoration of bowel continuity without the need for a permanent colostomy in many cases, significantly improving a patient’s quality of life post-surgery.
The decision to perform this type of anastomosis is carefully considered based on the tumor’s location, size, stage, and the patient’s overall health and sphincter function. It is a technically demanding procedure that requires significant surgical expertise to ensure both oncological clearance and optimal functional outcomes.
Procedure Steps for Side To End Coloanal Anastomosis
The Side to end coloanal anastomosis procedure steps involve several critical stages, typically performed under general anesthesia. The exact approach may vary depending on the surgeon’s preference and the patient’s specific condition, but generally includes:
- Bowel Preparation: Patients undergo a thorough bowel cleanse prior to surgery to minimize infection risk.
- Rectal Resection: The diseased portion of the rectum, along with surrounding lymph nodes, is carefully removed. This step is crucial for achieving clear surgical margins.
- Colon Mobilization: The remaining colon is mobilized and brought down into the pelvis to reach the anal canal without tension.
- Anastomosis Creation: The side of the mobilized colon is then meticulously sutured or stapled to the end of the anal canal, forming the new connection.
- Diverting Ostomy: In many cases, a temporary diverting ileostomy or colostomy is created in the abdominal wall. This diverts stool away from the newly formed anastomosis, allowing it to heal without contamination. The ostomy is typically reversed in a subsequent, less invasive procedure after several weeks or months.
The precision required during these steps is paramount to minimize complications and ensure effective long-term outcomes for the patient.
Recovery and Success Rates After Coloanal Anastomosis
The Side to end coloanal anastomosis recovery time varies among individuals but generally involves a hospital stay of 7 to 10 days, followed by a gradual return to normal activities over several weeks to months. Initial recovery focuses on pain management, monitoring for complications such as anastomotic leak or infection, and gradual reintroduction of diet. Patients often experience changes in bowel habits, including increased frequency, urgency, and sometimes incontinence, which typically improve over time as the body adapts to the new anatomy. Physical therapy and dietary adjustments are often recommended to aid in functional recovery.
Regarding Side to end coloanal anastomosis success rates, studies indicate favorable outcomes for both oncological control and functional preservation. For carefully selected patients, local recurrence rates for rectal cancer after this procedure are comparable to other rectal resection techniques. Success in preserving the anal sphincter and achieving satisfactory bowel function is high, with many patients regaining good to excellent continence. For instance, medical literature from specialized centers often reports success rates for sphincter preservation and local disease control exceeding 80-90% in appropriate candidates. However, it’s important to note that functional outcomes can continue to improve for up to a year or more after surgery, and some patients may experience persistent changes in bowel function. Regular follow-up with the surgical team is essential to monitor recovery and address any long-term concerns.