Hepatic Artery
The hepatic artery is a crucial blood vessel responsible for supplying oxygenated blood to the liver, a vital organ for numerous metabolic functions. Understanding its anatomy and function is essential for comprehending liver physiology and various medical conditions affecting this organ.
Key Takeaways
- The hepatic artery delivers oxygen-rich blood to the liver, complementing the portal vein’s nutrient supply.
- It originates from the celiac trunk and branches into the common, proper, and then right and left hepatic arteries within the liver.
- Its primary function is to sustain liver cells (hepatocytes) and the biliary system with oxygen and essential nutrients.
- Proper hepatic artery function is critical for liver metabolism, detoxification processes, and overall liver health.
- Disruptions to the hepatic artery can significantly impact liver viability and function.
What is the Hepatic Artery?
The Hepatic Artery is a major blood vessel that provides oxygenated blood to the liver, gallbladder, and parts of the stomach and pancreas. It is a critical component of the liver’s dual blood supply system, working in conjunction with the hepatic portal vein. While the portal vein delivers nutrient-rich, deoxygenated blood from the gastrointestinal tract, the hepatic artery ensures that the liver’s highly active metabolic cells receive a constant and adequate supply of oxygen and arterial nutrients necessary for their extensive functions, including detoxification, protein synthesis, and bile production.
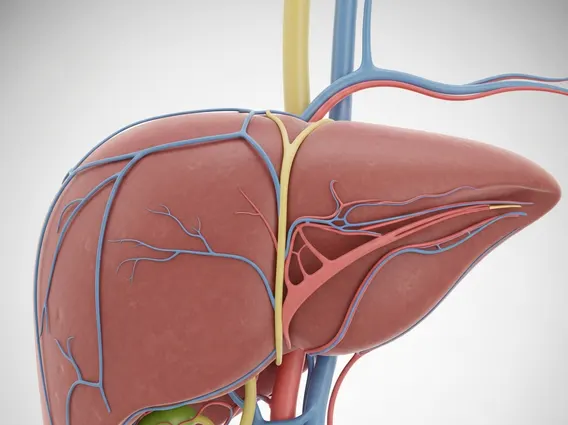
Hepatic Artery Anatomy and Blood Supply
The hepatic artery anatomy begins with its origin from the celiac trunk, which is the first major branch of the abdominal aorta. From the celiac trunk, it typically emerges as the common hepatic artery. This vessel then travels towards the liver, giving off branches to other organs before dividing into the gastroduodenal artery and the proper hepatic artery. The proper hepatic artery then ascends into the porta hepatis, the central fissure of the liver, where it typically divides into the right and left hepatic arteries, supplying the respective lobes of the liver. These branches further subdivide into smaller arterioles that penetrate the liver parenchyma, ensuring widespread distribution of oxygenated blood.
The hepatic artery blood supply is unique because the liver receives blood from two distinct sources, making it one of the most perfused organs in the body. Approximately 25-30% of the total blood flowing into the liver comes from the hepatic artery, while the remaining 70-75% is supplied by the hepatic portal vein. This dual supply is a vital compensatory mechanism; if one source is compromised, the other can often increase its flow to maintain liver viability. The oxygen saturation of the blood supplied by the hepatic artery is significantly higher than that from the portal vein, making it indispensable for the metabolic demands of hepatocytes.
Role and Function of the Hepatic Artery
The primary hepatic artery function is to deliver oxygen and arterial nutrients to the liver cells (hepatocytes) and the biliary tree. This oxygen supply is crucial for the liver’s high metabolic rate, supporting processes such as glucose metabolism, lipid synthesis, and the detoxification of various substances. Without an adequate arterial supply, hepatocytes would quickly suffer from hypoxia, leading to impaired function and potential cellular damage.
Beyond oxygenation, the hepatic artery also plays a significant role in:
- Maintaining Liver Viability: Essential for the survival and regeneration of liver tissue, particularly after injury or surgery.
- Supporting Biliary System: Supplies blood to the bile ducts, which are critical for transporting bile from the liver to the gallbladder and small intestine.
- Drug Metabolism: Ensures a steady supply of blood to the liver, where many medications and toxins are metabolized and detoxified.
- Interventional Procedures: It is a common target for therapeutic interventions, such as chemoembolization for liver tumors, where drugs are delivered directly to the tumor via the hepatic artery.
Disruptions to the hepatic artery, such as thrombosis or stenosis, can have severe consequences, potentially leading to liver ischemia, necrosis, and organ failure, underscoring its indispensable role in maintaining overall liver health and function.