Gamma Knife Therapy
Gamma Knife Therapy is an advanced form of stereotactic radiosurgery that delivers highly focused radiation to treat various brain conditions, including tumors, without the need for traditional incisions. This non-invasive approach offers a precise and effective treatment option for patients.
Key Takeaways
- Gamma Knife Therapy is a non-invasive radiosurgical treatment that uses precisely targeted radiation beams.
- It is primarily used to treat brain tumors, vascular malformations, and other neurological conditions.
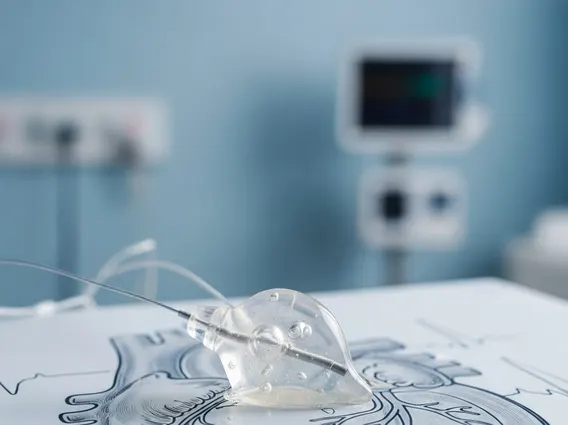
- The procedure involves a team of specialists, advanced imaging, and a specialized helmet to ensure pinpoint accuracy.
- Benefits include high precision, minimal recovery time, and reduced risk compared to open surgery.
- Potential risks are generally mild and temporary, such as localized swelling or fatigue.
What is Gamma Knife Therapy?
Gamma Knife Therapy is a highly precise form of stereotactic radiosurgery (SRS) that treats brain disorders using multiple beams of gamma radiation. Despite its name, there is no surgical knife involved; instead, it uses radiation to target and treat abnormalities within the brain with sub-millimeter accuracy. This advanced technique delivers a single, high dose of radiation to a specific target while minimizing exposure to surrounding healthy brain tissue. It is a well-established treatment, often performed on an outpatient basis, offering a less invasive alternative to traditional brain surgery for many patients.
The primary goal of Gamma Knife Therapy is to stop the growth of tumors or lesions, or to destroy them over time, by damaging the DNA of the abnormal cells. This causes the cells to gradually shrink or dissolve, improving symptoms and preventing further progression of the condition. The treatment is particularly effective for small to medium-sized lesions located deep within the brain or in areas that are difficult to access surgically.
How Gamma Knife Treatment Works for Brain Tumors
The Gamma Knife procedure for brain tumors involves a multidisciplinary team, including a neurosurgeon, radiation oncologist, and medical physicist. The process begins with the temporary placement of a lightweight frame on the patient’s head, which serves as a fiducial system for precise localization and immobilization during imaging and treatment. This frame ensures that the target within the brain can be identified with extreme accuracy.
Once the frame is in place, detailed imaging scans, such as magnetic resonance imaging (MRI), computed tomography (CT), or angiography, are performed. These images provide a three-dimensional map of the brain, allowing the medical team to precisely identify the target area, such as a brain tumor, and plan the radiation dose distribution. The planning phase is crucial, as it determines how the radiation beams will converge on the target while sparing healthy tissue.
During the treatment itself, the patient lies on a couch that slides into the Gamma Knife unit. The head frame is securely attached to the machine, ensuring that the target remains perfectly still. Up to 192 individual cobalt-60 gamma radiation sources are focused with extreme precision to deliver a concentrated dose of radiation to the target lesion. Each beam individually is too weak to harm healthy tissue, but where they converge, they deliver a powerful therapeutic dose. The entire treatment session typically lasts from a few minutes to several hours, depending on the size and shape of the target. Patients usually remain awake and comfortable throughout the procedure.
The steps involved in Gamma Knife treatment typically include:
- Frame Placement: A stereotactic head frame is temporarily attached to the patient’s head.
- Imaging: High-resolution MRI, CT, or angiogram scans are performed to pinpoint the target.
- Treatment Planning: A specialized software is used by the medical team to precisely map the radiation dose.
- Radiation Delivery: The patient is positioned in the Gamma Knife unit, and radiation is delivered to the target.
- Frame Removal: After treatment, the head frame is removed.
Benefits and Risks of Gamma Knife Therapy
Gamma Knife therapy benefits and risks are important considerations for patients and their healthcare providers. One of the most significant benefits is its non-invasive nature, meaning no surgical incision is required, which reduces the risk of infection and shortens recovery time. Patients often return home the same day and can resume normal activities quickly. The precision of the Gamma Knife system minimizes radiation exposure to surrounding healthy brain tissue, leading to fewer side effects compared to whole-brain radiation therapy or traditional surgery.
The procedure is also associated with a lower risk of hemorrhage and other complications often seen with open brain surgery. It can be a viable option for patients who are not candidates for conventional surgery due to age, general health, or the location of the lesion. According to the World Health Organization (WHO), non-communicable diseases, including cancers, are a leading cause of mortality globally, and advanced treatments like radiosurgery play a vital role in managing brain tumors.
However, like any medical procedure, Gamma Knife Therapy carries potential risks, although they are generally mild and temporary. Common side effects may include temporary swelling around the treated area, headache, nausea, or fatigue. In some cases, localized hair loss may occur. More serious, though rare, risks can include radiation-induced brain swelling, neurological deficits, or cyst formation, which may require further medical management. Patients are closely monitored after treatment to manage any potential side effects and assess the long-term efficacy of the therapy.