Mycosis Fungoides Plaque
Mycosis Fungoides Plaque represents a specific stage of Mycosis Fungoides, a rare and slow-growing type of non-Hodgkin lymphoma that primarily affects the skin. Understanding this condition is crucial for effective management and improved patient outcomes.
Key Takeaways
- Mycosis Fungoides Plaque is a manifestation of Mycosis Fungoides, a type of cutaneous T-cell lymphoma.
- It presents as distinct, raised, often reddish-brown skin lesions that can be itchy or scaly.
- Diagnosis typically involves a skin biopsy and specialized tests to identify abnormal T-cells.
- Treatment is individualized, often starting with skin-directed therapies, with systemic options for more advanced cases.
- The prognosis for early-stage Mycosis Fungoides Plaque is generally favorable, though it is a chronic condition requiring ongoing care.
What is Mycosis Fungoides Plaque?
Mycosis Fungoides Plaque refers to a particular stage in the progression of Mycosis Fungoides (MF), which is the most common form of cutaneous T-cell lymphoma (CTCL). This rare cancer originates from T-lymphocytes, a type of white blood cell, that primarily accumulate in the skin, forming lesions. Unlike many other lymphomas, MF typically progresses slowly over many years, often starting with patches before developing into plaques.
Plaques are distinct, elevated lesions that are often reddish-brown, irregular in shape, and can vary significantly in size. They may be itchy or scaly and can appear on any part of the body, though commonly found on areas not exposed to the sun, such as the buttocks or trunk. According to the National Cancer Institute, Mycosis Fungoides is the most common type of cutaneous T-cell lymphoma, with an estimated incidence of 0.3 to 0.5 cases per 100,000 persons per year in the United States, highlighting its rarity.
Mycosis Fungoides Plaque Symptoms, Causes, and Diagnosis
The presentation of mycosis fungoides plaque symptoms causes and its subsequent diagnosis are critical for timely intervention. The primary symptom is the appearance of the plaques themselves, which are typically:
- Elevated and firm to the touch
- Reddish-brown or purplish in color
- Often irregularly shaped
- Associated with itching (pruritus)
- Sometimes scaly or dry
These plaques can persist for months or years, and in some cases, they may spontaneously resolve or progress to more advanced stages, such as tumors or erythroderma. The exact causes of Mycosis Fungoides are not fully understood. It is believed to result from an abnormal proliferation of T-lymphocytes in the skin, driven by a complex interplay of genetic predispositions, environmental factors, and immune system dysregulation. It is important to note that Mycosis Fungoides is not contagious.
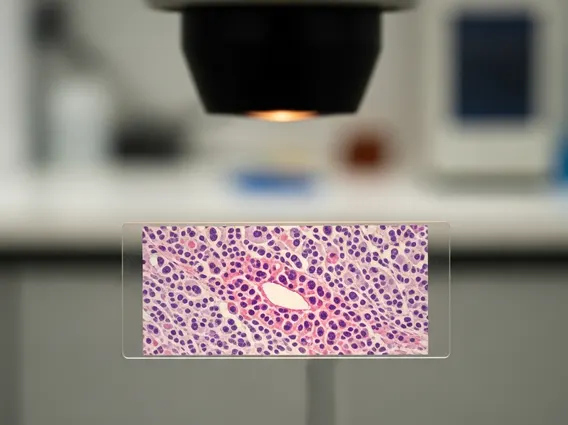
The process for mycosis fungoides plaque treatment diagnosis begins with a thorough physical examination of the skin. Definitive diagnosis relies heavily on a skin biopsy, where a small tissue sample is taken from a suspicious lesion and examined under a microscope by a dermatopathologist. This examination looks for characteristic features, such as atypical T-lymphocytes in the epidermis (epidermotropism). Additional specialized tests, including immunohistochemistry and T-cell receptor gene rearrangement studies, may be performed to confirm the clonality of the T-cells and rule out other skin conditions that mimic MF.
Treatment and Prognosis for Mycosis Fungoides Plaque
Treatment for Mycosis Fungoides Plaque is highly individualized, depending on the stage of the disease, the extent of skin involvement, and the patient’s overall health. The primary goal of treatment is to control symptoms, prevent disease progression, and improve quality of life. Early-stage Mycosis Fungoides Plaque is often managed with skin-directed therapies, which include:
- Topical corticosteroids to reduce inflammation and itching.
- Topical retinoids (e.g., bexarotene gel) to help normalize skin cell growth.
- Phototherapy, such as narrowband UVB or psoralen plus UVA (PUVA), which uses specific wavelengths of light to target affected skin cells.
For more extensive or resistant plaque disease, systemic therapies may be considered. These can include oral retinoids, interferon, methotrexate, or histone deacetylase inhibitors. In rare cases of advanced disease, chemotherapy or targeted therapies may be used. It is crucial for patients to work closely with a dermatologist or oncologist experienced in CTCL to develop the most appropriate treatment plan.
The mycosis fungoides plaque prognosis is generally favorable, particularly for individuals diagnosed in the early stages where the disease is confined to the skin. Many patients with early-stage Mycosis Fungoides Plaque can live for decades with appropriate management, and some may experience long periods of remission. However, it is a chronic condition that often requires ongoing monitoring and treatment to prevent progression. Prognosis can vary based on factors such as the extent of skin involvement, the presence of extracutaneous disease, and specific histopathological findings.