Secondary Ovarian Failure
Secondary Ovarian Failure is a complex endocrine condition characterized by the ovaries’ inability to function properly due to issues originating outside the ovaries themselves, typically involving the hypothalamus or pituitary gland. This article explores its definition, underlying causes, clinical presentation, and diagnostic approaches.
Key Takeaways
- Secondary Ovarian Failure results from impaired signaling from the brain (hypothalamus or pituitary) to the ovaries.
- Common causes include functional hypothalamic amenorrhea, pituitary tumors, and hyperprolactinemia.
- Key symptoms often involve menstrual irregularities, infertility, and signs of estrogen deficiency.
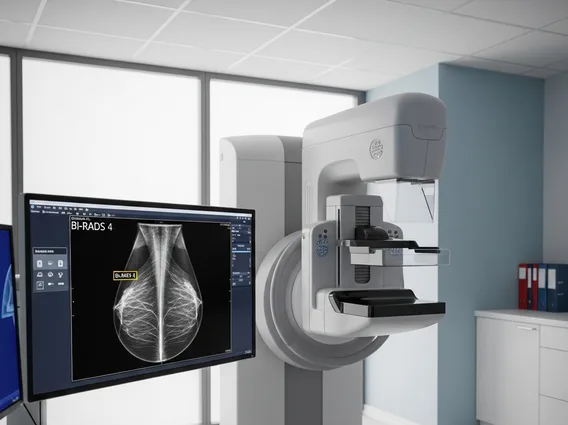
- Diagnosis relies on a combination of medical history, physical examination, and specific hormone tests, particularly low FSH and LH levels.
- Early and accurate diagnosis is crucial for managing symptoms and addressing potential underlying conditions.
What is Secondary Ovarian Failure?
Secondary Ovarian Failure refers to a condition where the ovaries, though structurally intact, fail to produce adequate hormones (primarily estrogen and progesterone) and eggs because they do not receive the necessary stimulating signals from the pituitary gland. This distinguishes it from primary ovarian failure, where the problem lies directly within the ovaries themselves. In secondary ovarian failure, the hypothalamic-pituitary-ovarian (HPO) axis is disrupted at the level of the hypothalamus or pituitary, leading to insufficient secretion of gonadotropin-releasing hormone (GnRH) from the hypothalamus or luteinizing hormone (LH) and follicle-stimulating hormone (FSH) from the pituitary gland. This lack of stimulation results in impaired follicular development and ovulation, impacting fertility and overall endocrine health.
Causes and Clinical Manifestations
The causes of secondary ovarian failure are diverse, stemming from disruptions in the intricate communication between the hypothalamus, pituitary gland, and ovaries. These disruptions can arise from various factors affecting either the hypothalamus or the pituitary gland. Understanding these underlying etiologies is crucial for effective management.
Common causes include:
- Functional Hypothalamic Amenorrhea (FHA): Often triggered by excessive physical exercise, significant psychological stress, or insufficient caloric intake (low body weight), leading to reduced GnRH pulsatility.
- Pituitary Tumors: Non-cancerous growths, such as prolactinomas, can interfere with the production of FSH and LH, or secrete excessive prolactin, which inhibits GnRH release.
- Sheehan’s Syndrome: A rare but severe condition involving pituitary gland damage due to massive blood loss during or after childbirth, leading to a deficiency of multiple pituitary hormones.
- Other Systemic Conditions: Chronic illnesses, severe nutritional deficiencies, or certain medications can also indirectly affect the HPO axis.
The symptoms of secondary ovarian failure primarily reflect the lack of ovarian hormone production. The most common clinical manifestation is amenorrhea, which is the absence of menstrual periods, or oligomenorrhea, characterized by infrequent periods. Women with this condition often experience infertility due to anovulation (lack of ovulation). Other symptoms can include those associated with estrogen deficiency, such as hot flashes, night sweats, vaginal dryness, reduced libido, and a decrease in bone mineral density over time, increasing the risk of osteoporosis. Depending on the underlying cause, additional symptoms like headaches or visual disturbances (in the case of pituitary tumors) may also be present.
Diagnosing Secondary Ovarian Failure
The secondary ovarian failure diagnosis process involves a comprehensive evaluation to differentiate it from other causes of menstrual irregularities and infertility. The initial steps include a detailed medical history, focusing on menstrual patterns, lifestyle factors, and any associated symptoms, followed by a thorough physical examination.
Key diagnostic tests involve hormone measurements:
Blood tests are essential to assess the levels of various hormones involved in the reproductive axis. Typically, in secondary ovarian failure, both FSH (follicle-stimulating hormone) and LH (luteinizing hormone) levels will be low or within the normal range, indicating insufficient stimulation from the pituitary gland. This contrasts with primary ovarian failure, where FSH and LH levels are characteristically high due to the pituitary gland’s attempt to stimulate non-responsive ovaries. Estradiol levels, a key ovarian hormone, are usually low, confirming the lack of ovarian activity. Prolactin levels are also measured to rule out hyperprolactinemia, a common cause of secondary ovarian failure. Additionally, thyroid function tests and other hormone assays may be performed to exclude other endocrine disorders that could mimic or contribute to the condition. Imaging studies, such as an MRI of the brain, are often utilized to evaluate the pituitary gland and hypothalamus for tumors or other structural abnormalities, especially if pituitary dysfunction is suspected.